Pelvic floor muscle training for female urinary incontinence: development of a programme theory from a longitudinal qualitative case study
- PMID: 39217312
- PMCID: PMC11365274
- DOI: 10.1186/s12905-024-03308-4
Pelvic floor muscle training for female urinary incontinence: development of a programme theory from a longitudinal qualitative case study
Abstract
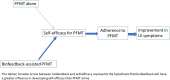
Background: Urinary incontinence (UI) negatively affects the well-being of women globally. Pelvic Floor Muscle Training (PFMT) is a complex intervention that aims to decrease UI symptoms. Information about how the multiple complex components involved in PFMT achieve and maintain the desired effect are rarely studied as a whole. The evidence base lacks data about how women experience PFMT over time and in the longer-term. This study explored women's experiences of biofeedback-assisted PFMT and PFMT alone, to identify and understand what influenced self-reported adherence to PFMT, and UI outcomes over time.
Methods: This rigorous longitudinal qualitative case study, nested within a randomised controlled trial, recruited forty cases (women with stress or mixed UI; 20 in biofeedback-assisted and 20 in PFMT alone group). A case included up to four semi-structured interviews with each woman (prior to starting PFMT, end of treatment [6 months], 12 months, 24 months). Analysis followed case study analytic traditions, resulting in a Programme Theory about PFMT from the perspectives of women with UI.
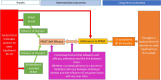
Findings: The theory demonstrates factors that motivated women to seek UI treatment, and how these influenced long-term adherence. Therapists who delivered PFMT played a crucial role in supporting women to know how to undertake PFMT (to have capability). Some, but not all, women developed self-efficacy for PFMT. Where women did not have PFMT self-efficacy, adherence tended to be poor. When women had PFMT self-efficacy, the conditions to support adherence were present, but contextual factors could still intercede to inhibit adherence. The intercession of contextual factors was individual to a woman and her life, meaning any particular contextual factor had inconsistent influences on PFMT adherence over time for individual women and exerted varying influences across different women.
Conclusion: Long term adherence to PFMT is a complex interaction between many different factors. Enquiring about an individual woman's motivation to seek treatment and understanding the contextual factors that affect an individual woman will enable a practitioner to support longer-term adherence.
Keywords: Adherence; Case study; Process evaluation; Programme theory; Qualitative; Self-efficacy; United Kingdom; Urinary incontinence.
© 2024. The Author(s).
Conflict of interest statement
The authors declare no competing interests.
Figures
Similar articles
-
Effectiveness and cost-effectiveness randomised controlled trial of basic versus biofeedback-mediated intensive pelvic floor muscle training for female stress or mixed urinary incontinence: protocol for the OPAL (optimising pelvic floor exercises to achieve long-term benefits) trial mixed methods longitudinal qualitative case study and process evaluation.BMJ Open. 2019 Feb 19;9(2):e024152. doi: 10.1136/bmjopen-2018-024152. BMJ Open. 2019. PMID: 30782894 Free PMC article.
-
Basic versus biofeedback-mediated intensive pelvic floor muscle training for women with urinary incontinence: the OPAL RCT.Health Technol Assess. 2020 Dec;24(70):1-144. doi: 10.3310/hta24700. Health Technol Assess. 2020. PMID: 33289476 Free PMC article. Clinical Trial.
-
Effectiveness of pelvic floor muscle training with and without electromyographic biofeedback for urinary incontinence in women: multicentre randomised controlled trial.BMJ. 2020 Oct 14;371:m3719. doi: 10.1136/bmj.m3719. BMJ. 2020. PMID: 33055247 Free PMC article. Clinical Trial.
-
Conservative interventions for treating urinary incontinence in women: an Overview of Cochrane systematic reviews.Cochrane Database Syst Rev. 2022 Sep 2;9(9):CD012337. doi: 10.1002/14651858.CD012337.pub2. Cochrane Database Syst Rev. 2022. PMID: 36053030 Free PMC article. Review.
-
Feedback or biofeedback to augment pelvic floor muscle training for urinary incontinence in women.Cochrane Database Syst Rev. 2011 Jul 6;(7):CD009252. doi: 10.1002/14651858.CD009252. Cochrane Database Syst Rev. 2011. PMID: 21735442 Review.
References
-
- Cardozo L, Rovner E, Wagg A, Wein A, Abrams P, editors. Incontinence. 7th ed. Bristol UK, International Continence Society; 2023.
-
- Toye F, Dixon S, Izett-Kay M, Keating S, McNiven A. Exploring the experiences of people with urogynaecology conditions in the UK: a reflexive thematic analysis and conceptual model. BMC Womens Health. 2023;23(1):431. 10.1186/s12905-023-02592-w. Published 2023 Aug 14. 10.1186/s12905-023-02592-w - DOI - PMC - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical