Case report: Identification of Hepatitis B Virus in the cerebrospinal fluid of neuromyelitis optica spectrum disorders and successful treatment with ofatumumab and inebilizumab
- PMID: 38426084
- PMCID: PMC10902669
- DOI: 10.3389/fimmu.2024.1351782
Case report: Identification of Hepatitis B Virus in the cerebrospinal fluid of neuromyelitis optica spectrum disorders and successful treatment with ofatumumab and inebilizumab
Abstract
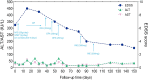
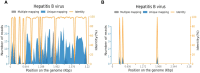
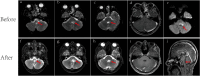
Neuromyelitis optica spectrum disorder (NMOSD) is a rare demyelinating disease of the central nervous system primarily affecting the optic nerves, spinal cord, and brainstem. Viral infection may trigger NMOSD. Here, we report the case of a 34-year-old female presenting with a range of symptoms including nausea, vomiting, dysphagia, choking, and fatigue with unsteady gait, diplopia, hearing loss, left-sided facial paralysis, breathing difficulties, and hoarseness of voice. Her HBV DNA concentration, as determined by quantitative PCR analysis, exceeded 5×107 IU/ml in serum and 4.48×102 IU/ml in CSF. Next-generation sequencing of CSF revealed 1,528 HBV sequences in DNA analysis and 6 sequences in RNA analysis. Serum aquaporin-4 antibody (AQP4-Ab) titer was 1:10, and the CSF titer was 1:3.2. Brain magnetic resonance imaging showed high signal intensities in the brain stem, medulla oblongata, and left middle cerebellar peduncle with mild restricted-diffusion. The patient received antiviral and hepatoprotective medications before the high-dose methylprednisolone pulse therapy. However, the patient did not respond well to the first-line treatment. Subsequently, the patient received ofatumumab and inebilizumab. Throughout the follow-up period, there was a gradual improvement in her neurological symptoms, with no reactivation of hepatitis B or deterioration of liver function observed. Thereby, to the best of our knowledge, we report the first case of successful treatment with ofatumumab and inebilizumab in a patient with NMOSD concurrent with HBV infection.
Keywords: case report; hepatitis B virus; inebilizumab; neuromyelitis optica spectrum disorders; ofatumumab.
Copyright © 2024 Cai, Liu, Zhou, Li, Zhou and Hong.
Conflict of interest statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Figures
Similar articles
-
Seropositive Neuromyelitis Optica in a Case of Undiagnosed Ankylosing Spondylitis: A Neuro-Rheumatological Conundrum.Qatar Med J. 2022 Jul 7;2022(3):29. doi: 10.5339/qmj.2022.29. eCollection 2022. Qatar Med J. 2022. PMID: 35864917 Free PMC article.
-
Safety and efficacy of inebilizumab for the treatment of neuromyelitis optica spectrum disorder: end-of-study results from the open-label period of the N-MOmentum trial.Lancet Neurol. 2024 Jun;23(6):588-602. doi: 10.1016/S1474-4422(24)00077-2. Lancet Neurol. 2024. PMID: 38760098 Clinical Trial.
-
Inebilizumab: A Review in Neuromyelitis Optica Spectrum Disorder.CNS Drugs. 2022 Oct;36(10):1133-1141. doi: 10.1007/s40263-022-00949-7. Epub 2022 Sep 7. CNS Drugs. 2022. PMID: 36070074 Free PMC article. Review.
-
Neuromyelitis optica spectrum disorder with active replication of hepatitis B virus and seropositive anti-aquaporin-4 antibody: A case report.Medicine (Baltimore). 2021 Sep 24;100(38):e27207. doi: 10.1097/MD.0000000000027207. Medicine (Baltimore). 2021. PMID: 34559109 Free PMC article.
-
Inebilizumab in AQP4-Ab-positive neuromyelitis optica spectrum disorder.Drugs Today (Barc). 2021 May;57(5):321-336. doi: 10.1358/dot.2021.57.5.3265453. Drugs Today (Barc). 2021. PMID: 34061127 Review.
References
-
- Liu J, Xu L, Chen ZL, Li M, Yi H, Peng FH. Comprehensive analysis of patients with neuromyelitis optica spectrum disorder (NMOSD) combined with chronic hepatitis B (CHB) infection and seropositive for anti-aquaporin-4 antibody. Bosn J Basic Med Sci (2018) 18(1):35–42. doi: 10.17305/bjbms.2017.2255 - DOI - PMC - PubMed
-
- Anamnart C, Tisavipat N, Owattanapanich W, Apiwattanakul M, Savangned P, Prayoonwiwat N, et al. . Newly diagnosed neuromyelitis optica spectrum disorders following vaccination: case report and systematic review. Mult Scler Relat Disord (2022) 58:103414. doi: 10.1016/j.msard.2021.103414 - DOI - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources

