Barriers and facilitators to implementation of evidence-based task-sharing mental health interventions in low- and middle-income countries: a systematic review using implementation science frameworks
- PMID: 35022081
- PMCID: PMC8756725
- DOI: 10.1186/s13012-021-01179-z
Barriers and facilitators to implementation of evidence-based task-sharing mental health interventions in low- and middle-income countries: a systematic review using implementation science frameworks
Abstract
Background: Task-sharing is a promising strategy to expand mental healthcare in low-resource settings, especially in low- and middle-income countries (LMICs). Research on how to best implement task-sharing mental health interventions, however, is hampered by an incomplete understanding of the barriers and facilitators to their implementation. This review aims to systematically identify implementation barriers and facilitators in evidence-based task-sharing mental health interventions using an implementation science lens, organizing factors across a novel, integrated implementation science framework.
Methods: PubMed, PsychINFO, CINAHL, and Embase were used to identify English-language, peer-reviewed studies using search terms for three categories: "mental health," "task-sharing," and "LMIC." Articles were included if they: focused on mental disorders as the main outcome(s); included a task-sharing intervention using or based on an evidence-based practice; were implemented in an LMIC setting; and included assessment or data-supported analysis of barriers and facilitators. An initial conceptual model and coding framework derived from the Consolidated Framework for Implementation Research and the Theoretical Domains Framework was developed and iteratively refined to create an integrated conceptual framework, the Barriers and Facilitators in Implementation of Task-Sharing Mental Health Interventions (BeFITS-MH), which specifies 37 constructs across eight domains: (I) client characteristics, (II) provider characteristics, (III) family and community factors, (IV) organizational characteristics, (V) societal factors, (VI) mental health system factors, (VII) intervention characteristics, and (VIII) stigma.
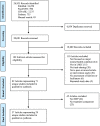
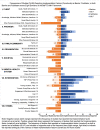
Results: Of the 26,935 articles screened (title and abstract), 192 articles underwent full-text review, yielding 37 articles representing 28 unique intervention studies that met the inclusion criteria. The most prevalent facilitators occur in domains that are more amenable to adaptation (i.e., the intervention and provider characteristics domains), while salient barriers occur in domains that are more challenging to modulate or intervene on-these include constructs in the client characteristics as well as the broader societal and structural levels of influence (i.e., the organizational, mental health system domains). Other notable trends include constructs in the family and community domains occurring as barriers and as facilitators roughly equally, and stigma constructs acting exclusively as barriers.
Conclusions: Using the BeFITS-MH model we developed based on implementation science frameworks, this systematic review provides a comprehensive identification and organization of barriers and facilitators to evidence-based task-sharing mental health interventions in LMICs. These findings have important implications for ongoing and future implementation of this critically needed intervention strategy, including the promise of leveraging task-sharing intervention characteristics as sites of continued innovation, the importance of but relative lack of engagement with constructs in macro-level domains (e.g., organizational characteristics, stigma), and the need for more delineation of strategies for task-sharing mental health interventions that researchers and implementers can employ to enhance implementation in and across levels.
Trial registration: PROSPERO CRD42020161357.
Keywords: Barriers and facilitators; Evidence-based practices; Implementation strategies; Low- and middle-income countries; Mental Health; Task-sharing.
© 2022. The Author(s).
Conflict of interest statement
The authors declare that they have no competing interests.
Figures

Similar articles
-
Conceptual framework on barriers and facilitators to implementing perinatal mental health care and treatment for women: the MATRIx evidence synthesis.Health Soc Care Deliv Res. 2024 Jan;12(2):1-187. doi: 10.3310/KQFE0107. Health Soc Care Deliv Res. 2024. PMID: 38317290
-
A case study of the development of a valid and pragmatic implementation science measure: the Barriers and Facilitators in Implementation of Task-Sharing Mental Health interventions (BeFITS-MH) measure.BMC Health Serv Res. 2024 Nov 6;24(1):1352. doi: 10.1186/s12913-024-11783-6. BMC Health Serv Res. 2024. PMID: 39501275 Free PMC article.
-
Beyond the black stump: rapid reviews of health research issues affecting regional, rural and remote Australia.Med J Aust. 2020 Dec;213 Suppl 11:S3-S32.e1. doi: 10.5694/mja2.50881. Med J Aust. 2020. PMID: 33314144
-
Barriers and facilitators of implementing interventions to improve appropriate antibiotic use in low- and middle-income countries: a systematic review based on the Consolidated Framework for Implementation Research.Implement Sci. 2022 May 12;17(1):30. doi: 10.1186/s13012-022-01209-4. Implement Sci. 2022. PMID: 35550169 Free PMC article. Review.
-
Barriers and facilitators of psychological help-seeking behaviors for perinatal women with depressive symptoms: A qualitative systematic review based on the Consolidated Framework for Implementation Research.Midwifery. 2023 Jul;122:103686. doi: 10.1016/j.midw.2023.103686. Epub 2023 Apr 21. Midwifery. 2023. PMID: 37119670 Review.
Cited by
-
One Size Does Not Fit All.Am J Geriatr Psychiatry. 2022 Jul;30(7):848-849. doi: 10.1016/j.jagp.2022.04.006. Epub 2022 Apr 20. Am J Geriatr Psychiatry. 2022. PMID: 35577654 Free PMC article. No abstract available.
-
A microcosting approach for planning and implementing community-based mental health prevention program: what does it cost?Health Econ Rev. 2024 May 21;14(1):35. doi: 10.1186/s13561-024-00510-w. Health Econ Rev. 2024. PMID: 38771498 Free PMC article.
-
A learning health systems approach to scaling up an evidence-based intervention for integrated primary mental healthcare case finding and referral in South Africa.BMJ Glob Health. 2024 Oct 22;9(10):e015165. doi: 10.1136/bmjgh-2024-015165. BMJ Glob Health. 2024. PMID: 39438070 Free PMC article.
-
Implementing Task-Shared Child and Adolescent Psychological Interventions in Low- and Middle-Income Countries: A Scoping Review.J Clin Child Adolesc Psychol. 2025 Jan-Feb;54(1):83-98. doi: 10.1080/15374416.2022.2151450. Epub 2022 Dec 12. J Clin Child Adolesc Psychol. 2025. PMID: 36507739 Review.
-
Piloting a community-based psychosocial group intervention designed to reduce distress among conflict-affected adults in Colombia: a mixed-method study of remote, hybrid, and in-person modalities during the COVID-19 pandemic.Int J Ment Health Syst. 2023 Oct 24;17(1):35. doi: 10.1186/s13033-023-00597-4. Int J Ment Health Syst. 2023. PMID: 37875939 Free PMC article.
References
-
- van Ginneken N, Tharyan P, Lewin S, Rao GN, Meera SM, Pian J, et al. Non-specialist health worker interventions for the care of mental, neurological and substance-abuse disorders in low- and middle-income countries. Cochrane Database Syst Rev. 2013:CD009149. 10.1002/14651858.CD009149.pub2. - PubMed
-
- Patel V, Saxena S, Lund C, Thornicroft G, Baingana F, Bolton P, et al. The Lancet Commission on global mental health and sustainable development. Lancet. 2018;392:1553–1598. - PubMed
-
- Raviola G, Naslund JA, Smith SL, Patel V. Innovative models in mental health delivery systems: task sharing care with non-specialist providers to close the mental health treatment gap. Curr Psychiatry Rep. 2019;21:44. - PubMed
-
- World Health Organization. WHO special initiative for mental health. https://www.who.int/initiatives/who-special-initiative-for-mental-health. Accessed 18 July 2021.
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

