High discrepancy in thrombotic events in non-small cell lung cancer patients with different genomic alterations
- PMID: 33889526
- PMCID: PMC8044490
- DOI: 10.21037/tlcr-20-1290
High discrepancy in thrombotic events in non-small cell lung cancer patients with different genomic alterations
Abstract
Background: Acute complications, such as venous thromboembolism (VTE), are common in patients with advanced severe lung cancers. However, current VTE risk scores cannot adequately identify high-risk patients with non-small cell lung cancer (NSCLC). The study proposed to elucidated the incidence of thromboembolism (TE) in patients with different oncogenic aberrations and the impact of these aberrations on the efficacy of targeted therapy in patients with NSCLC.
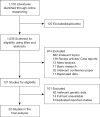
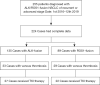
Methods: A systemic review was conducted in Web of Science, PubMed, Embase and the Cochrane Library to evaluate the incidence of TE in different molecular subtypes of NSCLC. Data from patients diagnosed of advanced NSCLC who harboring anaplastic lymphoma kinase (ALK) or ROS proto-oncogene 1 receptor tyrosine kinase (ROS1) rearrangements since 2016 to 2019 were also retrospectively collected. A meta-analysis with random-effects model, sensitivity analysis and publication bias were performed. The principal summary measure was incidence of thrombotic events in NSCLC patients. And the efficacy of tyrosine kinase inhibitor (TKI) therapy was compared between the two subgroups.
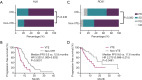
Results: A total of 5,767 cases from 20 studies were included in the analysis of the incidence of thrombosis in patients with different oncogenic alterations. The pooled analysis showed a higher risk of thrombosis in ROS1-fusion types (41%, 95% CI: 35-47%) and ALK-fusion types (30%, 95% CI: 24-37%) than in EGFR-mutation (12%, 95% CI: 8-17%), KRAS-mutation (25%, 95% CI: 13-50%), and wild-type (14%, 95% CI: 10-20%) cases. A high prevalence of thrombosis (ALK: 24.4%; ROS1: 32.6%) was observed in the Shanghai Pulmonary Hospital (SPH) cohort of 224 patients with ALK or ROS1 fusion. Furthermore, patients with embolism had significantly shorter progression-free survival (PFS) after TKI therapy than those without embolism, both in the ALK+ cohort (5.6 vs. 12.9 months, P<0.0001) and in the ROS1+ cohort (9.6 vs. 17.6 months, P=0.0481).
Conclusions: NSCLC patients with ALK/ROS1 rearrangements are more likely to develop thrombosis than patients with other oncogenic alterations. Thrombosis may also be associated with an inferior response and PFS after TKI therapy.
Keywords: Non-small cell lung cancer (NSCLC); ROS1; anaplastic lymphoma kinase (ALK); thromboembolism (TE).
2021 Translational Lung Cancer Research. All rights reserved.
Conflict of interest statement
Conflicts of Interest: All authors have completed the ICMJE uniform disclosure form (available at http://dx.doi.org/10.21037/tlcr-20-1290). CZ has served as an unpaid editorial board member of Translational Lung Cancer Research from Aug 2020 to Jul 2022. The other authors have no conflicts of interest to declare.
Figures


Similar articles
-
Risk of thromboembolism in non-small-cell lung cancers patients with different oncogenic drivers, including ROS1, ALK, and EGFR mutations.ESMO Open. 2022 Dec;7(6):100742. doi: 10.1016/j.esmoop.2022.100742. Epub 2022 Dec 6. ESMO Open. 2022. PMID: 36493600 Free PMC article.
-
Thromboembolism in ALK+ and ROS1+ NSCLC patients: A systematic review and meta-analysis.Lung Cancer. 2021 Jul;157:147-155. doi: 10.1016/j.lungcan.2021.05.019. Epub 2021 May 20. Lung Cancer. 2021. PMID: 34049720
-
Clinical features and therapeutic options in non-small cell lung cancer patients with concomitant mutations of EGFR, ALK, ROS1, KRAS or BRAF.Cancer Med. 2019 Jun;8(6):2858-2866. doi: 10.1002/cam4.2183. Epub 2019 Apr 24. Cancer Med. 2019. PMID: 31016879 Free PMC article.
-
Efficacy of immunotherapy in patients with oncogene-driven non-small-cell lung cancer: a systematic review and meta-analysis.Ther Adv Med Oncol. 2024 Feb 27;16:17588359231225036. doi: 10.1177/17588359231225036. eCollection 2024. Ther Adv Med Oncol. 2024. PMID: 38420602 Free PMC article. Review.
-
Targeted therapies in non-small cell lung cancer: a focus on ALK/ROS1 tyrosine kinase inhibitors.Expert Rev Anticancer Ther. 2018 Jan;18(1):71-80. doi: 10.1080/14737140.2018.1412260. Epub 2017 Dec 6. Expert Rev Anticancer Ther. 2018. PMID: 29187012 Review.
Cited by
-
Risk Factors and Prediction Models for Venous Thromboembolism in Ambulatory Patients with Lung Cancer.Healthcare (Basel). 2021 Jun 21;9(6):778. doi: 10.3390/healthcare9060778. Healthcare (Basel). 2021. PMID: 34205695 Free PMC article. Review.
-
The association between ROS1 rearrangement and risk of thromboembolic events in patients with advanced non-small cell lung cancer: a multicenter study in China.Thromb J. 2022 Sep 27;20(1):56. doi: 10.1186/s12959-022-00417-8. Thromb J. 2022. PMID: 36167545 Free PMC article.
-
Therapeutic Strategies Focused on Cancer-Associated Hypercoagulation for Ovarian Clear Cell Carcinoma.Cancers (Basel). 2022 Apr 24;14(9):2125. doi: 10.3390/cancers14092125. Cancers (Basel). 2022. PMID: 35565252 Free PMC article. Review.
-
Thromboembolic Events Associated with Epidermal Growth Factor Receptor Tyrosine Kinase Inhibitors: A Pharmacovigilance Analysis of the US FDA Adverse Event Reporting System (FAERS) Database.Clin Drug Investig. 2024 Mar;44(3):199-207. doi: 10.1007/s40261-024-01346-2. Epub 2024 Feb 20. Clin Drug Investig. 2024. PMID: 38376794 Review.
-
Osimertinib for an Advanced NSCLC Patient with Two Common EGFR Mutations and a Concomitant MET Exon 14 Skipping Mutation: A Case Report.Cancer Manag Res. 2023 Jul 12;15:645-650. doi: 10.2147/CMAR.S412199. eCollection 2023. Cancer Manag Res. 2023. PMID: 37465082 Free PMC article.
References
LinkOut - more resources
Full Text Sources
Other Literature Sources
Research Materials
Miscellaneous
