Exploring the Clinical and Genetic Spectrum of Steroid Resistant Nephrotic Syndrome: The PodoNet Registry
- PMID: 30065916
- PMCID: PMC6057105
- DOI: 10.3389/fped.2018.00200
Exploring the Clinical and Genetic Spectrum of Steroid Resistant Nephrotic Syndrome: The PodoNet Registry
Abstract
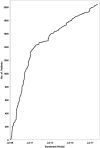
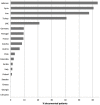
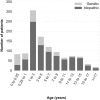
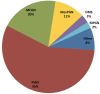
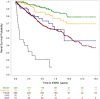
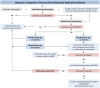
Background: Steroid resistant nephrotic syndrome (SRNS) is a rare condition, accounting for 10-15% of all children with idiopathic nephrotic syndrome. SRNS can be caused by genetic abnormalities or immune system dysfunction. The prognosis of SRNS varies from permanent remission to progression to end-stage kidney disease, and post-transplant recurrence is common. Objectives: The PodoNet registry project aims to explore the demographics and phenotypes of immune-mediated and genetic forms of childhood SRNS, to assess genotype-phenotype correlations, to evaluate clinical management and long-term outcomes, and to search for novel genetic entities and diagnostic and prognostic biomarkers in SRNS. Methods: In 2009, an international registry for SRNS was established to collect retro- and prospective information on renal and extrarenal disease manifestations, histopathological and genetic findings and information on family history, pharmacotherapy responsiveness and long-term outcomes. To date, more than 2,000 patients have been enrolled at 72 pediatric nephrology centers, constituting the largest pediatric SRNS cohort assembled to date. Results: In the course of the project, traditional Sanger sequencing was replaced by NGS-based gene panel screening covering over 30 podocyte-related genes complemented by whole exome sequencing. These approaches allowed to establish genetic diagnoses in 24% of the patients screened, widened the spectrum of genetic disease entities presenting with SRNS phenotype (COL4A3-5, CLCN5), and contributed to the discovery of new disease causing genes (MYOE1, PTPRO). Forty two percent of patients responded to intensified immunosuppression with complete or partial remission of proteinuria, whereas 58% turned out multi-drug resistant. Medication responsiveness was highly predictive of a favorable long-term outcome, whereas the diagnosis of genetic disease was associated with a high risk to develop end-stage renal disease during childhood. Genetic SRNS forms were generally resistant to immunosuppressive treatment, justifying to avoid such pharmacotherapies altogether once a genetic diagnosis is established. Even symptomatic anti-proteinuric treatment with RAS antagonists seems to be challenging and of limited efficacy in genetic forms of SRNS. The risk of post-transplant disease recurrence was around 30% in non-genetic SRNS whereas it is negligible in genetic cases. Conclusion: In summary, the PodoNet Registry has collected detailed clinical and genetic information in a large SRNS cohort and continues to generate fundamental insights regarding demographic and etiological disease aspects, genotype-phenotype associations, the efficacy of therapeutic strategies, and long-term patient and renal outcomes including post-transplant disease recurrence.
Keywords: NPHS2; SRNS; WT1; nephrotic syndrome; steroid resistant nephrotic syndrome.
Figures
Similar articles
-
Spectrum of steroid-resistant and congenital nephrotic syndrome in children: the PodoNet registry cohort.Clin J Am Soc Nephrol. 2015 Apr 7;10(4):592-600. doi: 10.2215/CJN.06260614. Epub 2015 Jan 29. Clin J Am Soc Nephrol. 2015. PMID: 25635037 Free PMC article.
-
Genomic and clinical profiling of a national nephrotic syndrome cohort advocates a precision medicine approach to disease management.Kidney Int. 2017 Apr;91(4):937-947. doi: 10.1016/j.kint.2016.10.013. Epub 2017 Jan 20. Kidney Int. 2017. PMID: 28117080
-
Outcomes of steroid-resistant nephrotic syndrome in children not treated with intensified immunosuppression.Pediatr Nephrol. 2023 May;38(5):1499-1511. doi: 10.1007/s00467-022-05762-4. Epub 2022 Oct 31. Pediatr Nephrol. 2023. PMID: 36315273 Free PMC article.
-
Management of Steroid-Resistant Nephrotic Syndrome in Children.Cureus. 2021 Nov 8;13(11):e19363. doi: 10.7759/cureus.19363. eCollection 2021 Nov. Cureus. 2021. PMID: 34925975 Free PMC article. Review.
-
Genetic tests in children with steroid-resistant nephrotic syndrome.Kidney Res Clin Pract. 2020 Mar 31;39(1):7-16. doi: 10.23876/j.krcp.20.001. Kidney Res Clin Pract. 2020. PMID: 32155690 Free PMC article. Review.
Cited by
-
Rare heterozygous variants in paediatric steroid resistant nephrotic syndrome - a population-based analysis of their significance.Sci Rep. 2024 Aug 10;14(1):18568. doi: 10.1038/s41598-024-68837-2. Sci Rep. 2024. PMID: 39127776 Free PMC article.
-
Hereditable variants of classical protein tyrosine phosphatase genes: Will they prove innocent or guilty?Front Cell Dev Biol. 2023 Jan 23;10:1051311. doi: 10.3389/fcell.2022.1051311. eCollection 2022. Front Cell Dev Biol. 2023. PMID: 36755664 Free PMC article. Review.
-
Current understandings in treating children with steroid-resistant nephrotic syndrome.Pediatr Nephrol. 2021 Apr;36(4):747-761. doi: 10.1007/s00467-020-04476-9. Epub 2020 Feb 21. Pediatr Nephrol. 2021. PMID: 32086590 Free PMC article. Review.
-
Outcomes of children with idiopathic steroid resistant nephrotic syndrome: a single centre observational study.J Bras Nefrol. 2023 Apr-Jun;45(2):199-209. doi: 10.1590/2175-8239-JBN-2022-0073en. J Bras Nefrol. 2023. PMID: 36179014 Free PMC article.
-
CoQ10-related sustained remission of proteinuria in a child with COQ6 glomerulopathy-a case report.Pediatr Nephrol. 2018 Dec;33(12):2383-2387. doi: 10.1007/s00467-018-4083-3. Epub 2018 Sep 19. Pediatr Nephrol. 2018. PMID: 30232548 Free PMC article.
References
Publication types
LinkOut - more resources
Full Text Sources
Other Literature Sources

