A clinical approach to the diagnosis of patients with leukodystrophies and genetic leukoencephelopathies
- PMID: 25655951
- PMCID: PMC4390485
- DOI: 10.1016/j.ymgme.2014.12.434
A clinical approach to the diagnosis of patients with leukodystrophies and genetic leukoencephelopathies
Abstract
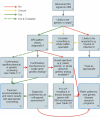
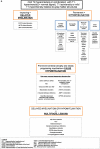
Leukodystrophies (LD) and genetic leukoencephalopathies (gLE) are disorders that result in white matter abnormalities in the central nervous system (CNS). Magnetic resonance (MR) imaging (MRI) has dramatically improved and systematized the diagnosis of LDs and gLEs, and in combination with specific clinical features, such as Addison's disease in Adrenoleukodystrophy or hypodontia in Pol-III related or 4H leukodystrophy, can often resolve a case with a minimum of testing. The diagnostic odyssey for the majority LD and gLE patients, however, remains extensive--many patients will wait nearly a decade for a definitive diagnosis and at least half will remain unresolved. The combination of MRI, careful clinical evaluation and next generation genetic sequencing holds promise for both expediting the diagnostic process and dramatically reducing the number of unresolved cases. Here we present a workflow detailing the Global Leukodystrophy Initiative (GLIA) consensus recommendations for an approach to clinical diagnosis, including salient clinical features suggesting a specific diagnosis, neuroimaging features and molecular genetic testing. We also discuss recommendations on the use of broad-spectrum next-generation sequencing in instances of ambiguous MRI or clinical findings. We conclude with a proposal for systematic trials of genome-wide agnostic testing as a first line diagnostic in LDs and gLEs given the increasing number of genes associated with these disorders.
Keywords: Glia; Leukodystrophy; Myelin.
Published by Elsevier Inc.
Figures

Similar articles
-
An update on clinical, pathological, diagnostic, and therapeutic perspectives of childhood leukodystrophies.Expert Rev Neurother. 2020 Jan;20(1):65-84. doi: 10.1080/14737175.2020.1699060. Epub 2019 Dec 12. Expert Rev Neurother. 2020. PMID: 31829048 Review.
-
Update on leukodystrophies and developing trials.J Neurol. 2024 Jan;271(1):593-605. doi: 10.1007/s00415-023-11996-5. Epub 2023 Sep 27. J Neurol. 2024. PMID: 37755460 Free PMC article. Review.
-
Leukodystrophies underlying cryptic spastic paraparesis: frequency and phenotype in 76 patients.Eur J Neurol. 2014 Jul;21(7):983-8. doi: 10.1111/ene.12423. Epub 2014 Apr 2. Eur J Neurol. 2014. PMID: 24698313
-
Etiologic Spectrum of Pediatric-Onset Leukodystrophies and Genetic Leukoencephalopathies: The Five-Year Experience of a Tertiary Care Center in Southern India.Pediatr Neurol. 2024 Mar;152:130-152. doi: 10.1016/j.pediatrneurol.2023.12.027. Epub 2024 Jan 3. Pediatr Neurol. 2024. PMID: 38277958
-
Tools for diagnosis of leukodystrophies and other disorders presenting with white matter disease.Curr Neurol Neurosci Rep. 2005 Mar;5(2):110-8. doi: 10.1007/s11910-005-0008-1. Curr Neurol Neurosci Rep. 2005. PMID: 15743548 Review.
Cited by
-
Adulthood leukodystrophies.Nat Rev Neurol. 2018 Feb;14(2):94-105. doi: 10.1038/nrneurol.2017.175. Epub 2018 Jan 5. Nat Rev Neurol. 2018. PMID: 29302065 Free PMC article. Review.
-
Inherited paediatric neurometabolic disorders, can brain magnetic resonance imaging predict?Neurosciences (Riyadh). 2020 Oct;25(5):392-398. doi: 10.17712/nsj.2020.5.20200072. Neurosciences (Riyadh). 2020. PMID: 33459289 Free PMC article.
-
POLR3-Related Leukodystrophy: Exploring Potential Therapeutic Approaches.Front Cell Neurosci. 2021 Jan 28;14:631802. doi: 10.3389/fncel.2020.631802. eCollection 2020. Front Cell Neurosci. 2021. PMID: 33633543 Free PMC article.
-
Disease specific therapies in leukodystrophies and leukoencephalopathies.Mol Genet Metab. 2015 Apr;114(4):527-36. doi: 10.1016/j.ymgme.2015.01.014. Epub 2015 Feb 7. Mol Genet Metab. 2015. PMID: 25684057 Free PMC article.
-
Practical Approaches and Knowledge Gaps in the Care for Children With Leukodystrophies.J Child Neurol. 2021 Jan;36(1):65-78. doi: 10.1177/0883073820946154. Epub 2020 Sep 2. J Child Neurol. 2021. PMID: 32875938 Free PMC article. Review.
References
-
- Vanderver A, Tonduti D, Schiffmann R, Schmidt J, Van der Knaap MS. Leukodys-trophy overview. In: Pagon RA, Adam MP, Bird TD, Dolan CR, Fong CT, Smith RJH, Stephens K, editors. GeneReviews(R) University of Washington, Seattle University of Washington; Seattle: 2014. All rights reserved., Seattle (WA) - PubMed
-
- Vanderver A, Prust M, Tonduti D, Mochel F, Hussey H, Helman G, Garbern J, Eichler F, Labauge P, Aubourg P, Rodriguez D, Patterson M, Van Hove J, Schmidt J, Wolf N, Boespflug-Tanguy O, Schiffmann R, van der Knaap M. Case definition and classification of leukodystrophies and leukoencephalopathies. Mol. Genet. Metab. 2014 in press. - PMC - PubMed
-
- Heim P, Claussen M, Hoffmann B, Conzelmann E, Gärtner J, Harzer K, Hunneman DH, Köhler W, Kurlemann G, Kohlschütter A. Leukodystrophy incidence in Germany. Am. J. Med. Genet. 1997;71:475–478. - PubMed
-
- Bernard G, Vanderver A. Pol III-related leukodystrophies. 2012
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Research Materials
