Staphylococcus aureus screening and decolonization in orthopaedic surgery and reduction of surgical site infections
- PMID: 23463284
- PMCID: PMC3676622
- DOI: 10.1007/s11999-013-2875-0
Staphylococcus aureus screening and decolonization in orthopaedic surgery and reduction of surgical site infections
Abstract
Background: Staphylococcus aureus is the most common organism responsible for orthopaedic surgical site infections (SSIs). Patients who are carriers for methicillin-sensitive S. aureus or methicillin-resistant S. aureus (MRSA) have a higher likelihood of having invasive S. aureus infections. Although some have advocated screening for S. aureus and decolonizing it is unclear whether these efforts reduce SSIs.
Questions/purposes: The purposes of this study were to determine (1) whether S. aureus screening and decolonization reduce SSIs in orthopaedic patients and (2) if implementing this protocol is cost-effective.
Methods: Studies for this systematic review were identified by searching PubMed, which includes MEDLINE (1946-present), EMBASE.com (1974-present), and the Cochrane Library's (John Wiley & Sons) Cochrane Database of Systematic Reviews (CDSR), Cochrane Central Register of Controlled Trials (CENTRAL), Database of Abstracts of Reviews of Effects (DARE), Health Technology Assessment Database (HTAD), and the NHS Economic Evaluation Database (NHSEED). Comprehensive literature searches were developed using EMTREE, MeSH, and keywords for each of the search concepts of decolonization, MRSA, and orthopedics/orthopedic surgery. Studies published before 1968 were excluded. We analyzed 19 studies examining the ability of the decolonization protocol to reduce SSIs and 10 studies detailing the cost-effectiveness of S. aureus screening and decolonization.
Results: All 19 studies showed a reduction in SSIs or wound complications by instituting a S. aureus screening and decolonization protocol in elective orthopaedic (total joints, spine, and sports) and trauma patients. The S. aureus screening and decolonization protocol also saved costs in orthopaedic patients when comparing the costs of screening and decolonization with the reduction of SSIs.
Conclusions: Preoperative screening and decolonization of S. aureus in orthopaedic patients is a cost-effective means to reduce SSIs.
Level of evidence: Level IV, systematic review of Level I-IV studies. See the Guidelines for Authors for a complete description of levels of evidence.
Figures
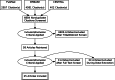
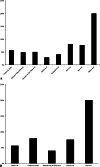

Comment in
-
Reply to the Letter to the editor: Staphylococcus aureus screening and decolonization in orthopaedic surgery and reduction of surgical site infections.Clin Orthop Relat Res. 2013 Nov;471(11):3712-3. doi: 10.1007/s11999-013-3255-5. Epub 2013 Aug 28. Clin Orthop Relat Res. 2013. PMID: 23982407 Free PMC article. No abstract available.
-
Letter to the editor: Staphylococcus aureus screening and decolonization in orthopaedic surgery and reduction of surgical site infections.Clin Orthop Relat Res. 2013 Nov;471(11):3709-11. doi: 10.1007/s11999-013-3254-6. Epub 2013 Sep 7. Clin Orthop Relat Res. 2013. PMID: 24014267 Free PMC article. No abstract available.
Similar articles
-
Impact of preoperative MRSA screening and decolonization on hospital-acquired MRSA burden.Clin Orthop Relat Res. 2013 Jul;471(7):2367-71. doi: 10.1007/s11999-013-2848-3. Epub 2013 Feb 20. Clin Orthop Relat Res. 2013. PMID: 23423618 Free PMC article.
-
Letter to the editor: Staphylococcus aureus screening and decolonization in orthopaedic surgery and reduction of surgical site infections.Clin Orthop Relat Res. 2013 Nov;471(11):3709-11. doi: 10.1007/s11999-013-3254-6. Epub 2013 Sep 7. Clin Orthop Relat Res. 2013. PMID: 24014267 Free PMC article. No abstract available.
-
Reply to the Letter to the editor: Staphylococcus aureus screening and decolonization in orthopaedic surgery and reduction of surgical site infections.Clin Orthop Relat Res. 2013 Nov;471(11):3712-3. doi: 10.1007/s11999-013-3255-5. Epub 2013 Aug 28. Clin Orthop Relat Res. 2013. PMID: 23982407 Free PMC article. No abstract available.
-
Pre-surgical Nasal Decolonization of Staphylococcus aureus: A Health Technology Assessment.Ont Health Technol Assess Ser. 2022 Aug 23;22(4):1-165. eCollection 2022. Ont Health Technol Assess Ser. 2022. PMID: 36160757 Free PMC article. Review.
-
Methicillin-resistant Staphylococcus aureus (MRSA): colonisation and pre-operative screening.Bone Joint J. 2013 Jan;95-B(1):4-9. doi: 10.1302/0301-620X.95B1.27973. Bone Joint J. 2013. PMID: 23307666 Review.
Cited by
-
Evidence-Based Bundled Quality Improvement Intervention for Reducing Surgical Site Infection in Lower Extremity Vascular Bypass Procedures.J Am Coll Surg. 2019 Jan;228(1):44-53. doi: 10.1016/j.jamcollsurg.2018.10.002. Epub 2018 Oct 22. J Am Coll Surg. 2019. PMID: 30359836 Free PMC article.
-
Implications for diagnosis and treatment of peri-spinal implant infections from experiences in periprosthetic joint infections-a literature comparison and review.J Spine Surg. 2020 Dec;6(4):800-813. doi: 10.21037/jss-20-12. J Spine Surg. 2020. PMID: 33447686 Free PMC article. Review.
-
Hospital Cost of Staphylococcal Infection after Cardiothoracic or Orthopedic Operations in France: A Retrospective Database Analysis.Surg Infect (Larchmt). 2015 Aug;16(4):428-35. doi: 10.1089/sur.2014.045. Epub 2015 Jun 2. Surg Infect (Larchmt). 2015. PMID: 26207403 Free PMC article.
-
Use of surveillance data to identify target populations for Staphylococcus aureus vaccines and prevent surgical site infections: a pilot study.Hum Vaccin Immunother. 2014;10(12):3517-21. doi: 10.4161/21645515.2014.979625. Hum Vaccin Immunother. 2014. PMID: 25668663 Free PMC article.
-
Use of Chlorhexidine Preparations in Total Joint Arthroplasty.J Bone Jt Infect. 2017 Jan 1;2(1):15-22. doi: 10.7150/jbji.16934. eCollection 2017. J Bone Jt Infect. 2017. PMID: 28529860 Free PMC article. Review.
References
-
- Berthelot P, Grattard F, Cazorla C, Passot JP, Fayard JP, Meley R, Bejuy J, Farizon F, Pozzetto B, Lucht F. Is nasal carriage of Staphylococcus aureus the main acquisition pathway for surgical-site infection in orthopaedic surgery? Eur J Clin Microbiol Infect Dis. 2010;29:373–382. doi: 10.1007/s10096-009-0867-5. - DOI - PubMed
-
- Bode LG, Kluytmans JA, Wertheim HF, Bogaers D, Vandenbroucke-Grauls CM, Roosendaal R, Troelstra A, Box AT, Voss A, van der Tweel I, van Belkum A, Verbrugh HA, Vos MC. Preventing surgical-site infections in nasal carriers of Staphylococcus aureus. N Engl J Med. 2010;362:9–17. doi: 10.1056/NEJMoa0808939. - DOI - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Research Materials

