Onset of progressive phase is an age-dependent clinical milestone in multiple sclerosis
- PMID: 22736750
- PMCID: PMC4029334
- DOI: 10.1177/1352458512451510
Onset of progressive phase is an age-dependent clinical milestone in multiple sclerosis
Abstract
Background: It is unclear if all patients with relapsing-remitting multiple sclerosis (RRMS) ultimately develop progressive MS. Onset of progressive disease course seems to be age- rather than disease duration-dependent. Some forms of progressive MS (e.g. primary progressive MS (PPMS)) are uncommon in population-based studies. Ascertainment of patients with PPMS from clinic-based populations can facilitate a powerful comparison of age at progression onset between secondary progressive MS (SPMS) and PPMS but may introduce unclear biases.
Objective: Our aim is to confirm that onset of progressive disease course is more relevant to the patient's age than the presence or duration of a pre-progression relapsing disease course in MS.
Methods: We studied a population-based MS cohort (n=210, RRMS n=109, progressive MS n=101) and a clinic-based progressive MS cohort (n=754). Progressive course was classified as primary (PPMS; n=322), single attack (SAPMS; n=112) and secondary progressive (SPMS; n=421). We studied demographics (chi(2) or t-test), age-of-progression-onset (t-test) and time to Expanded Disability Status Scale of 6 (EDSS6) (Kaplan-Meier analyses).
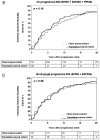
Results: Sex ratio (p=0.58), age at progression onset (p=0.37) and time to EDSS6 (p=0.16) did not differ between the cohorts. Progression had developed before age 75 in 99% of patients with known progressive disease course; 38% with RRMS did not develop progression by age 75. Age at progression onset did not differ between SPMS (44.9±9.6), SAPMS (45.5±9.6) and PPMS (45.7±10.8). In either cohort, only 2% of patients had reached EDSS6 before onset of progression.
Conclusions: Patients with RRMS do not inevitably develop a progressive disease course. Onset of progression is more dependent on age than the presence or duration of a pre-progression symptomatic disease course. Moderate disability is sustained predominantly after the onset of a progressive disease course in MS.
Conflict of interest statement
Figures



Similar articles
-
Preferential spinal cord volume loss in primary progressive multiple sclerosis.Mult Scler. 2019 Jun;25(7):947-957. doi: 10.1177/1352458518775006. Epub 2018 May 21. Mult Scler. 2019. PMID: 29781383
-
Clinically relevant cranio-caudal patterns of cervical cord atrophy evolution in MS.Neurology. 2019 Nov 12;93(20):e1852-e1866. doi: 10.1212/WNL.0000000000008466. Epub 2019 Oct 14. Neurology. 2019. PMID: 31611336
-
Multiple sclerosis by phenotype in Germany.Mult Scler Relat Disord. 2022 Jan;57:103326. doi: 10.1016/j.msard.2021.103326. Epub 2021 Oct 10. Mult Scler Relat Disord. 2022. PMID: 35158442
-
Pathogenic Mechanisms Associated With Different Clinical Courses of Multiple Sclerosis.Front Immunol. 2019 Jan 10;9:3116. doi: 10.3389/fimmu.2018.03116. eCollection 2018. Front Immunol. 2019. PMID: 30687321 Free PMC article. Review.
-
Primary progressive multiple sclerosis: part of the MS disease spectrum or separate disease entity?Acta Neuropathol. 2012 May;123(5):627-38. doi: 10.1007/s00401-012-0953-0. Epub 2012 Feb 11. Acta Neuropathol. 2012. PMID: 22327362 Review.
Cited by
-
Aging-Exacerbated Acute Axon and Myelin Injury Is Associated with Microglia-Derived Reactive Oxygen Species and Is Alleviated by the Generic Medication Indapamide.J Neurosci. 2020 Oct 28;40(44):8587-8600. doi: 10.1523/JNEUROSCI.1098-20.2020. Epub 2020 Oct 15. J Neurosci. 2020. PMID: 33060175 Free PMC article.
-
Intense inflammation and nerve damage in early multiple sclerosis subsides at older age: a reflection by cerebrospinal fluid biomarkers.PLoS One. 2013 May 7;8(5):e63172. doi: 10.1371/journal.pone.0063172. Print 2013. PLoS One. 2013. PMID: 23667585 Free PMC article.
-
Impact of trial design and patient heterogeneity on the identification of clinically effective therapies for progressive MS.Mult Scler. 2018 Dec;24(14):1795-1807. doi: 10.1177/1352458518800800. Epub 2018 Oct 10. Mult Scler. 2018. PMID: 30303445 Free PMC article.
-
Impact of aging on treatment considerations for multiple sclerosis patients.Front Neurol. 2023 Jul 7;14:1197212. doi: 10.3389/fneur.2023.1197212. eCollection 2023. Front Neurol. 2023. PMID: 37483447 Free PMC article. Review.
-
Greater sensitivity to multiple sclerosis disability worsening and progression events using a roving versus a fixed reference value in a prospective cohort study.Mult Scler. 2018 Jun;24(7):963-973. doi: 10.1177/1352458517709619. Epub 2017 May 30. Mult Scler. 2018. PMID: 28554238 Free PMC article.
References
-
- Kantarci OH, Weinshenker BG. Natural history of multiple sclerosis. Neurologic Clinics. 2005;23(1):17–38. - PubMed
-
- Confavreux C, Vukusic S. Natural history of multiple sclerosis: a unifying concept. Brain. 2006;129(Pt 3):606–16. - PubMed
-
- Lublin FD, Reingold SC. Defining the clinical course of multiple sclerosis: results of an international survey. National Multiple Sclerosis Society (USA) Advisory Committee on Clinical Trials of New Agents in Multiple Sclerosis. Neurology. 1996;46(4):907–11. - PubMed
-
- Wolinsky JS. The diagnosis of primary progressive multiple sclerosis. Journal of the neurological sciences. 2003;206(2):145–52. - PubMed
-
- Kremenchutzky M, Rice GP, Baskerville J, Wingerchuk DM, Ebers GC. The natural history of multiple sclerosis: a geographically based study 9: observations on the progressive phase of the disease. Brain. 2006;129(Pt 3):584–94. - PubMed
Publication types
MeSH terms
Grants and funding
- R01 NS032129/NS/NINDS NIH HHS/United States
- U01NS 45719/NS/NINDS NIH HHS/United States
- R01 NS058698/NS/NINDS NIH HHS/United States
- P50 NS038667/NS/NINDS NIH HHS/United States
- R01 NS048357/NS/NINDS NIH HHS/United States
- UL1 RR024150/RR/NCRR NIH HHS/United States
- 2P50NS038667-11/NS/NINDS NIH HHS/United States
- U01 NS045719/NS/NINDS NIH HHS/United States
- R01 NS065829/NS/NINDS NIH HHS/United States
- R01 NS060881/NS/NINDS NIH HHS/United States
- R01 NS 49577-6/NS/NINDS NIH HHS/United States
- R01 NS 58698/NS/NINDS NIH HHS/United States
- R01 NS058698-01A2/NS/NINDS NIH HHS/United States
- UL1 RR 24150-2/RR/NCRR NIH HHS/United States
- R01 NS65829/NS/NINDS NIH HHS/United States
- R01 NS049577/NS/NINDS NIH HHS/United States
- R21 NS073684/NS/NINDS NIH HHS/United States
- R01 GM092993/GM/NIGMS NIH HHS/United States
- R01 NS 60881/NS/NINDS NIH HHS/United States
- R01 NS060881-01A209/NS/NINDS NIH HHS/United States
- R01 NS024180/NS/NINDS NIH HHS/United States
LinkOut - more resources
Full Text Sources
Medical

