Alexander disease: diagnosis with MR imaging
- PMID: 11237983
- PMCID: PMC7976831
Alexander disease: diagnosis with MR imaging
Abstract
Background and purpose: To date, the demonstration of Rosenthal fibers on brain biopsy or autopsy specimens is considered a prerequisite for a definitive diagnosis of Alexander disease. We initiated a multiinstitutional survey of MR abnormalities in both presumed and confirmed cases of Alexander disease to assess the possibility of an MR-based diagnosis.
Methods: MR imaging studies in three patients with an autopsy-based diagnosis of Alexander disease were analyzed to define MR criteria for the diagnosis. These criteria were then applied to 217 children with leukoencephalopathy of unknown origin.
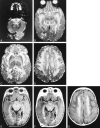
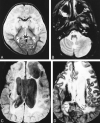
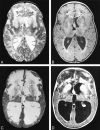
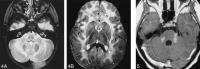
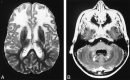
Results: Five MR imaging criteria were defined: extensive cerebral white matter changes with frontal predominance, a periventricular rim with high signal on T1-weighted images and low signal on T2-weighted images, abnormalities of basal ganglia and thalami, brain stem abnormalities, and contrast enhancement of particular gray and white matter structures. Four of the five criteria had to be met for an MR imaging-based diagnosis. In a retrospective analysis of the MR studies of the 217 patients, 19 were found who fulfilled these criteria. No other essentially new MR abnormalities were found in these patients. In four of the 19 patients, subsequent histologic confirmation was obtained. The clinical symptomatology was the same in the patients with and without histologic confirmation and correlated well with the MR abnormalities. MR abnormalities were in close agreement with the known histopathologic findings of Alexander disease.
Conclusion: The defined criteria are sufficient for an in vivo MR imaging diagnosis of Alexander disease; only in atypical cases is a brain biopsy still necessary for a definitive diagnosis.
Figures
Similar articles
-
Diffusion-weighted MR imaging of global cerebral anoxia.AJNR Am J Neuroradiol. 1999 Jun-Jul;20(6):999-1007. AJNR Am J Neuroradiol. 1999. PMID: 10445435 Free PMC article.
-
Early cerebral images of Alexander disease: report of one case.Acta Paediatr Taiwan. 2004 Jan-Feb;45(1):52-5. Acta Paediatr Taiwan. 2004. PMID: 15264709
-
Alexander disease: early presence of cerebral MRI criteria.Eur J Paediatr Neurol. 2009 Nov;13(6):556-8. doi: 10.1016/j.ejpn.2008.11.008. Epub 2009 Jan 6. Eur J Paediatr Neurol. 2009. PMID: 19128991
-
Diffusion-weighted MR of the brain: methodology and clinical application.Radiol Med. 2005 Mar;109(3):155-97. Radiol Med. 2005. PMID: 15775887 Review. English, Italian.
-
Differential diagnosis for bilateral abnormalities of the basal ganglia and thalamus.Radiographics. 2011 Jan-Feb;31(1):5-30. doi: 10.1148/rg.311105041. Radiographics. 2011. PMID: 21257930 Review.
Cited by
-
Pathology of the neurovascular unit in leukodystrophies.Acta Neuropathol Commun. 2021 Jun 3;9(1):103. doi: 10.1186/s40478-021-01206-6. Acta Neuropathol Commun. 2021. PMID: 34082828 Free PMC article.
-
Megalencephalic leukoencephalopathy with subcortical cysts in all three siblings of a non-Aggarwal Indian family.Ann Indian Acad Neurol. 2012 Jul;15(3):214-7. doi: 10.4103/0972-2327.99723. Ann Indian Acad Neurol. 2012. PMID: 22919198 Free PMC article.
-
Infantile Alexander Disease with Late Onset Infantile Spasms and Hypsarrhythmia.Balkan J Med Genet. 2019 Dec 21;22(2):77-82. doi: 10.2478/bjmg-2019-0017. eCollection 2019 Dec. Balkan J Med Genet. 2019. PMID: 31942421 Free PMC article.
-
Neuroimaging and clinical features in type II (late-onset) Alexander disease.Neurology. 2014 Jan 7;82(1):49-56. doi: 10.1212/01.wnl.0000438230.33223.bc. Epub 2013 Dec 4. Neurology. 2014. PMID: 24306001 Free PMC article.
-
CSF and Blood Levels of GFAP in Alexander Disease.eNeuro. 2015 Oct 1;2(5):ENEURO.0080-15.2015. doi: 10.1523/ENEURO.0080-15.2015. eCollection 2015 Sep. eNeuro. 2015. PMID: 26478912 Free PMC article.
References
-
- Alexander WS. Progressive fibrinoid degeneration of fibrillary astrocytes associated with mental retardation in a hydrocephalic child. Brain 1949;72:373-381 - PubMed
-
- Crome L. Megalencephaly associated with hyaline neuropathy. Brain 1953;76:215-228 - PubMed
-
- Wohlwill FJ, Bernstein J, Yakovlev PI. Dysmyelogenic leukodystrophy. J Neuropathol Exp Neurol 1959;18:359-383 - PubMed
-
- Holland IM, Kendall BE. Computed tomography in Alexander's disease. Neuroradiology 1980;20:103-106 - PubMed
-
- Towfighi J, Young R, Sassani J, Ramer J, Horoupian DS. Alexander's disease: further light- and electron-microscopic observations. Acta Neuropathol 1983;61:36-42 - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Miscellaneous
