Long-Term Survivorship of Cervical Spine Procedures; A Survivorship Meta-Analysis and Meta-Regression
- PMID: 36069054
- PMCID: PMC10240585
- DOI: 10.1177/21925682221125766
Long-Term Survivorship of Cervical Spine Procedures; A Survivorship Meta-Analysis and Meta-Regression
Abstract
Study design: Systematic Review.
Objectives: To conduct a meta-analysis on the survivorship of commonly performed cervical spine procedures to develop survival function curves for (i) second surgery at any cervical level, and (ii) adjacent level surgery.
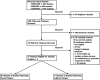
Methods: A systematic review of was conducted following PRISMA guidelines. Articles with cohorts of greater than 20 patients followed for a minimum of 36 months and with available survival data were included. Procedures included were anterior cervical discectomy and fusion (ACDF), cervical disc arthroplasty (ADR), laminoplasty (LAMP), and posterior laminectomy and fusion (PDIF). Reconstructed individual patient data were pooled across studies using parametric Bayesian survival meta-regression.
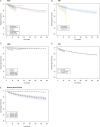
Results: Of 1829 initial titles, 16 citations were included for analysis. 73 811 patients were included in the second surgery analysis and 2858 patients in the adjacent level surgery analysis. We fit a Log normal accelerated failure time model to the second surgery data and a Gompertz proportional hazards model to the adjacent level surgery data. Relative to ACDF, the risk of second surgery was higher with ADR and PDIF with acceleration factors 1.73 (95% CrI: 1.04, 2.80) and 1.35 (95% CrI: 1.25, 1.46) respectively. Relative to ACDF, the risk of second surgery was lower with LAMP with deceleration factor .06 (95% CrI: .05, .07). ADR decreased the risk of adjacent level surgery with hazard ratio .43 (95% CrI: .33, .55).
Conclusions: In cases of clinical equipoise between fusion procedures, our analysis suggests superior survivorship with anterior procedures. For all procedures, laminoplasty demonstrated superior survivorship.
Keywords: anterior cervical discectomy and fusion; cervical disc arthroplasty; degenerative cervical myelopathy; survivorship curve.
Conflict of interest statement
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Figures
Similar articles
-
Is cervical disc arthroplasty good for congenital cervical stenosis?J Neurosurg Spine. 2017 May;26(5):577-585. doi: 10.3171/2016.10.SPINE16317. Epub 2017 Mar 10. J Neurosurg Spine. 2017. PMID: 28291414
-
Long-term clinical and radiographic outcomes of the Prestige LP artificial cervical disc replacement at 2 levels: results from a prospective randomized controlled clinical trial.J Neurosurg Spine. 2017 Jul;27(1):7-19. doi: 10.3171/2016.11.SPINE16746. Epub 2017 Apr 7. J Neurosurg Spine. 2017. PMID: 28387616 Clinical Trial.
-
Cervical disc arthroplasty versus anterior cervical discectomy and fusion: a meta-analysis of rates of adjacent-level surgery to 7-year follow-up.J Spine Surg. 2020 Mar;6(1):217-232. doi: 10.21037/jss.2019.12.09. J Spine Surg. 2020. PMID: 32309660 Free PMC article.
-
Kinematics of the cervical adjacent segments after disc arthroplasty compared with anterior discectomy and fusion: a systematic review and meta-analysis.Spine (Phila Pa 1976). 2012 Oct 15;37(22 Suppl):S85-95. doi: 10.1097/BRS.0b013e31826d6628. Spine (Phila Pa 1976). 2012. PMID: 22885834 Review.
-
Anterior cervical discectomy and fusion versus posterior laminoplasty for multilevel cervical myelopathy: A meta-analysis.Int J Surg. 2017 Dec;48:247-253. doi: 10.1016/j.ijsu.2017.06.030. Epub 2017 Jul 5. Int J Surg. 2017. PMID: 28687344 Review.
Cited by
-
Nonoperative Care Versus Surgery for Degenerative Cervical Myelopathy: An Application of a Health Economic Technique to Simulate Head-to-Head Comparisons.JB JS Open Access. 2024 Nov 21;9(4):e23.00166. doi: 10.2106/JBJS.OA.23.00166. eCollection 2024 Oct-Dec. JB JS Open Access. 2024. PMID: 39574781 Free PMC article.
-
Treatment decision-making factors among patients with cervical myelopathy: a discrete-choice experiment.J Patient Rep Outcomes. 2024 Nov 11;8(1):129. doi: 10.1186/s41687-024-00810-z. J Patient Rep Outcomes. 2024. PMID: 39527291 Free PMC article.
-
Treatment of the two-level degenerative cervical disk diseases based on algorithmic anterior approach: a multicenter prospective study.Neurosurg Rev. 2023 Sep 18;46(1):247. doi: 10.1007/s10143-023-02157-3. Neurosurg Rev. 2023. PMID: 37723281
References
-
- Fehlings MG, Tetreault LA, Riew KD, et al. A clinical practice guideline for the management of patients with degenerative cervical myelopathy: Recommendations for patients with mild, moderate, and severe disease and nonmyelopathic patients with evidence of cord compression. Global Spine Journal. 2017;7(3_supplement):70S-83S. doi:10.1177/2192568217701914 - DOI - PMC - PubMed
LinkOut - more resources
Full Text Sources
Research Materials