Telephone interventions for symptom management in adults with cancer
- PMID: 32483832
- PMCID: PMC7264015
- DOI: 10.1002/14651858.CD007568.pub2
Telephone interventions for symptom management in adults with cancer
Abstract
Background: People with cancer experience a variety of symptoms as a result of their disease and the therapies involved in its management. Inadequate symptom management has implications for patient outcomes including functioning, psychological well-being, and quality of life (QoL). Attempts to reduce the incidence and severity of cancer symptoms have involved the development and testing of psycho-educational interventions to enhance patients' symptom self-management. With the trend for care to be provided nearer patients' homes, telephone-delivered psycho-educational interventions have evolved to provide support for the management of a range of cancer symptoms. Early indications suggest that these can reduce symptom severity and distress through enhanced symptom self-management.
Objectives: To assess the effectiveness of telephone-delivered interventions for reducing symptoms associated with cancer and its treatment. To determine which symptoms are most responsive to telephone interventions. To determine whether certain configurations (e.g. with/without additional support such as face-to-face, printed or electronic resources) and duration/frequency of intervention calls mediate observed cancer symptom outcome effects.
Search methods: We searched the following databases: the Cochrane Central Register of Controlled Trials (CENTRAL; 2019, Issue 1); MEDLINE via OVID (1946 to January 2019); Embase via OVID (1980 to January 2019); (CINAHL) via Athens (1982 to January 2019); British Nursing Index (1984 to January 2019); and PsycINFO (1989 to January 2019). We searched conference proceedings to identify published abstracts, as well as SIGLE and trial registers for unpublished studies. We searched the reference lists of all included articles for additional relevant studies. Finally, we handsearched the following journals: Cancer, Journal of Clinical Oncology, Psycho-oncology, Cancer Practice, Cancer Nursing, Oncology Nursing Forum, Journal of Pain and Symptom Management, and Palliative Medicine. We restricted our search to publications published in English.
Selection criteria: We included randomised controlled trials (RCTs) and quasi-RCTs that compared one or more telephone interventions with one other, or with other types of interventions (e.g. a face-to-face intervention) and/or usual care, with the stated aim of addressing any physical or psychological symptoms of cancer and its treatment, which recruited adults (over 18 years) with a clinical diagnosis of cancer, regardless of tumour type, stage of cancer, type of treatment, and time of recruitment (e.g. before, during, or after treatment).
Data collection and analysis: We used Cochrane methods for trial selection, data extraction and analysis. When possible, anxiety, depressive symptoms, fatigue, emotional distress, pain, uncertainty, sexually-related and lung cancer symptoms as well as secondary outcomes are reported as standardised mean differences (SMDs) with 95% confidence intervals (CIs), and we presented a descriptive synthesis of study findings. We reported on findings according to symptoms addressed and intervention types (e.g. telephone only, telephone combined with other elements). As many studies included small samples, and because baseline scores for study outcomes often varied for intervention and control groups, we used change scores and associated standard deviations. The certainty of the evidence for each outcome was interpreted using the Grading of Recommendations Assessment, Development and Evaluation (GRADE) approach.
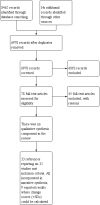
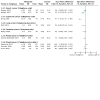
Main results: Thirty-two studies were eligible for inclusion; most had moderate risk of bias,often related to blinding. Collectively, researchers recruited 6250 people and studied interventions in people with a variety of cancer types and across the disease trajectory, although many participants had breast cancer or early-stage cancer and/or were starting treatment. Studies measured symptoms of anxiety, depression, emotional distress, uncertainty, fatigue, and pain, as well as sexually-related symptoms and general symptom intensity and/or distress. Interventions were primarily delivered by nurses (n = 24), most of whom (n = 16) had a background in oncology, research, or psychiatry. Ten interventions were delivered solely by telephone; the rest combined telephone with additional elements (i.e. face-to-face consultations and digital/online/printed resources). The number of calls delivered ranged from 1 to 18; most interventions provided three or four calls. Twenty-one studies provided evidence on effectiveness of telephone-delivered interventions and the majority appeared to reduce symptoms of depression compared to control. Nine studies contributed quantitative change scores (CSs) and associated standard deviation results (or these could be calculated). Likewise, many telephone interventions appeared effective when compared to control in reducing anxiety (16 studies; 5 contributed quantitative CS results); fatigue (9 studies; 6 contributed to quantitative CS results); and emotional distress (7 studies; 5 contributed quantitative CS results). Due to significant clinical heterogeneity with regards to interventions introduced, study participants recruited, and outcomes measured, meta-analysis was not conducted. For other symptoms (uncertainty, pain, sexually-related symptoms, dyspnoea, and general symptom experience), evidence was limited; similarly meta-analysis was not possible, and results from individual studies were largely conflicting, making conclusions about their management through telephone-delivered interventions difficult to draw. Heterogeneity was considerable across all trials for all outcomes. Overall, the certainty of evidence was very low for all outcomes in the review. Outcomes were all downgraded due to concerns about overall risk of bias profiles being frequently unclear, uncertainty in effect estimates and due to some inconsistencies in results and general heterogeneity. Unsubstantiated evidence suggests that telephone interventions in some capacity may have a place in symptom management for adults with cancer. However, in the absence of reliable and homogeneous evidence, caution is needed in interpreting the narrative synthesis. Further, there were no clear patterns across studies regarding which forms of interventions (telephone alone versus augmented with other elements) are most effective. It is impossible to conclude with any certainty which forms of telephone intervention are most effective in managing the range of cancer-related symptoms that people with cancer experience.
Authors' conclusions: Telephone interventions provide a convenient way of supporting self-management of cancer-related symptoms for adults with cancer. These interventions are becoming more important with the shift of care closer to patients' homes, the need for resource/cost containment, and the potential for voluntary sector providers to deliver healthcare interventions. Some evidence supports the use of telephone-delivered interventions for symptom management for adults with cancer; most evidence relates to four commonly experienced symptoms - depression, anxiety, emotional distress, and fatigue. Some telephone-delivered interventions were augmented by combining them with face-to-face meetings and provision of printed or digital materials. Review authors were unable to determine whether telephone alone or in combination with other elements provides optimal reduction in symptoms; it appears most likely that this will vary by symptom. It is noteworthy that, despite the potential for telephone interventions to deliver cost savings, none of the studies reviewed included any form of health economic evaluation. Further robust and adequately reported trials are needed across all cancer-related symptoms, as the certainty of evidence generated in studies within this review was very low, and reporting was of variable quality. Researchers must strive to reduce variability between studies in the future. Studies in this review are characterised by clinical and methodological diversity; the level of this diversity hindered comparison across studies. At the very least, efforts should be made to standardise outcome measures. Finally, studies were compromised by inclusion of small samples, inadequate concealment of group allocation, lack of observer blinding, and short length of follow-up. Consequently, conclusions related to symptoms most amenable to management by telephone-delivered interventions are tentative.
Copyright © 2020 The Cochrane Collaboration. Published by John Wiley & Sons, Ltd.
Conflict of interest statement
Emma Ream: principal investigator of a trial that assessed the effectiveness of a telephone intervention for cancer patients experiencing fatigue. Amanda Amanda Euesden Hughes: none known. Anna Cox: none known. Katy Skarparis: none known. Alison Richardson: none known. Vibe H Pedersen: none known. Theresa Wiseman: none known. Angus Forbes: none known. Andrew Bryant: none known.
Figures





Update of
- doi: 10.1002/14651858.CD007568
Similar articles
-
Educational interventions for the management of cancer-related fatigue in adults.Cochrane Database Syst Rev. 2016 Nov 24;11(11):CD008144. doi: 10.1002/14651858.CD008144.pub2. Cochrane Database Syst Rev. 2016. PMID: 27883365 Free PMC article. Review.
-
Behavioural modification interventions for medically unexplained symptoms in primary care: systematic reviews and economic evaluation.Health Technol Assess. 2020 Sep;24(46):1-490. doi: 10.3310/hta24460. Health Technol Assess. 2020. PMID: 32975190 Free PMC article.
-
Early palliative care for adults with advanced cancer.Cochrane Database Syst Rev. 2017 Jun 12;6(6):CD011129. doi: 10.1002/14651858.CD011129.pub2. Cochrane Database Syst Rev. 2017. PMID: 28603881 Free PMC article. Review.
-
Music interventions for improving psychological and physical outcomes in people with cancer.Cochrane Database Syst Rev. 2021 Oct 12;10(10):CD006911. doi: 10.1002/14651858.CD006911.pub4. Cochrane Database Syst Rev. 2021. PMID: 34637527 Free PMC article. Review.
-
Music interventions for improving psychological and physical outcomes in cancer patients.Cochrane Database Syst Rev. 2016 Aug 15;(8):CD006911. doi: 10.1002/14651858.CD006911.pub3. Cochrane Database Syst Rev. 2016. Update in: Cochrane Database Syst Rev. 2021 Oct 12;10:CD006911. doi: 10.1002/14651858.CD006911.pub4. PMID: 27524661 Updated. Review.
Cited by
-
Models of Integration of Specialized Palliative Care with Oncology.Curr Treat Options Oncol. 2021 Apr 8;22(5):44. doi: 10.1007/s11864-021-00836-1. Curr Treat Options Oncol. 2021. PMID: 33830352 Free PMC article. Review.
-
Palliative care models for patients living with advanced cancer: a narrative review for the emergency department clinician.Emerg Cancer Care. 2022;1(1):10. doi: 10.1186/s44201-022-00010-9. Epub 2022 Aug 5. Emerg Cancer Care. 2022. PMID: 35966217 Free PMC article. Review.
-
Self-care behaviors in patients with cancer treated with oral anticancer agents: a systematic review.Support Care Cancer. 2022 Oct;30(10):8465-8483. doi: 10.1007/s00520-022-07166-4. Epub 2022 May 31. Support Care Cancer. 2022. PMID: 35639188 Review.
-
Patient reported outcomes in oncology: changing perspectives-a systematic review.Health Qual Life Outcomes. 2022 May 21;20(1):82. doi: 10.1186/s12955-022-01987-x. Health Qual Life Outcomes. 2022. PMID: 35597948 Free PMC article. Review.
-
Impact of COVID-19 on older adults with cancer and their caregivers' cancer treatment experiences study: The ICE-OLD study.PLoS One. 2023 Sep 20;18(9):e0291756. doi: 10.1371/journal.pone.0291756. eCollection 2023. PLoS One. 2023. PMID: 37729131 Free PMC article.
References
References to studies included in this review
Allard 2007 {published data only}
-
- Allard N. Day surgery for breast cancer: effects of a psychoeducational telephone intervention on functional status and emotional distress. Oncology Nursing Forum 2007;34(1):133-41. - PubMed
Allen 2002 {published data only}
-
- Allen S, Shah A, Nezu A, Nezu C, Ciambrone D, Hogan J, et al. A problem-solving approach to stress reduction among younger women with breast carcinoma: a randomized controlled trial. Cancer 2002;94(12):3089-100. - PubMed
Badger 2005 {published data only}
-
- Badger T, Segrin C, Meek P, Lopez A, Bonham E, Sieger A. Telephone interpersonal counseling with women with breast cancer: symptom management and quality of life. Oncology Nursing Forum 2005;32:273-9. - PubMed
Badger 2007 {published data only}
-
- Badger T, Segrin C, Dorros S, Meek P, Lopez A. Depression and anxiety in women with breast cancer and their partners. Nursing Research 2007;56:44-53. - PubMed
Badger 2013a {published data only}
-
- Badger T, Segrin C, Pasvogel A, Lopez AM. The effect of psychosocial interventions delivered by telephone and videophone on quality of life in early-stage breast cancer survivors and their supportive partners. Journal of Telemedicine and Telecare 2013;19(5):260-5. - PubMed
Badger 2013b {published data only}
-
- Badger T, Segrin C, Hepworth J, Pasvogel A, Weihs K, Lopez A. Telephone-delivered health education and interpersonal counseling improve quality of life for Latinas with breast cancer and their supportive partners. Psycho-Oncology 2012;22(5):1035–42. - PubMed
Badr 2015 {published data only}
Bailey 2004 {published data only}
-
- Bailey D, Mishel M, Belyea M, Stewart J, Mohler J. Uncertainty intervention for watchful waiting in prostate cancer. Cancer Nursing 2004;27:339-46. - PubMed
Barsevick 2004 {published data only}
-
- Barsevick A, Dudley W, Beck S, Sweeney C, Whitmer K, Nail L. A randomized clinical trial of energy conservation for patients with cancer-related fatigue. Cancer 2004;100(6):1302–10. - PubMed
Barsevick 2010 {published data only}
Chambers 2014 {published data only}
-
- Chambers S, Girgis A, Occhipinti S, Hutchison S, Turner J, Mcdowell M, et al. A randomised trial comparing two low-intensity psychological interventions for distressed patients with cancer and their caregivers. Oncology Nursing Forum 2014;41(4):E256-66. - PubMed
Chambers 2015 {published data only}
-
- Chambers SK, Occhipinti S, Schover L, Nielson L, Zajglewicz L, Clutton S. A randomised controlled trial of a couples-based sexuality intervention for men with localised prostate cancer and their female partners. Psycho-oncology 2015;24(7):748-56. - PubMed
Dong 2018 {published data only}
-
- Dong X, Sun G, ZhanJ, Liu F, Ma S, Li P, et al. Telephone-based reminiscence therapy for colorectal cancer patients undergoing postoperative chemotherapy complicated with depression: a three-arm randomised controlled trial. Supportive Care in Cancer 2018;DOI: 10.1007/s00520-018-4566-6:1-9. - PubMed
Downe‐Wamboldt 2007 {published data only}
-
- Downe-Wamboldt B, Butler L, Melanson P, Coulter L, Singleton J, Keefe J, et al. The effects and expense of augmenting usual cancer clinic care with telephone problem-solving counseling. Cancer Nursing 2007;30(6):441-53. - PubMed
Girgis 2009 {published data only}
-
- Girgis A, Breen S, Stacey F, Lecathelinais C. Impact of two supportive care interventions on anxiety, depression, quality of life, and unmet needs in patients with nonlocalized breast and colorectal cancers. Journal of Clinical Oncology 2009;27(36):6180-90. - PubMed
Kroenke 2010 {published data only}
Livingston 2010 {published data only}
-
- Livingston P, White V, Hayman J, Maunsell E, Dunn S, Hill D. The psychological impact of a specialist referral and telephone intervention on male cancer patients: a randomised controlled trial. Psycho-oncology 2010;19(6):617–25. - PubMed
Mishel 2002 {published data only}
-
- Mishel M, Belyea M, Germino B, Stewart J, Balley JR D, Robertson C, et al. Helping patients with localized prostate carcinoma manage uncertainty and treatment side effects: nurse-delivered psychoeducational intervention over the telephone. Cancer 2002;94(6):1854-66. - PubMed
Mishel 2005 {published data only}
-
- Mishel M, Germino B, Gil K, Belyea M, Laney I, Stewart J, et al. Benefits from an uncertainty management intervention for African-American and Caucasian older long-term breast cancer survivors. Psycho-oncology 2005;14(11):962-78. - PubMed
Molassiotis 2009 {published data only}
-
- Molassiotis A, Brearley S, Saunders M, Craven O, Wardley A, Farrell C, et al. Effectiveness of a home care nursing program in the symptom management of patients with colorectal and breast cancer receiving oral chemotherapy: a randomized, controlled trial. Journal of Clinical Oncology 2009;27(36):6191-8. - PubMed
Mosher 2016 {published data only}
Porter 2011 {published data only}
Rawl 2002 {published data only}
-
- Rawl S, Given B, Given C, Champion V, Kozachik S, Barton D, et al. Intervention to improve psychological functioning for newly diagnosed patients with cancer. Oncology Nursing Forum Online 2002;29(6):967-75. - PubMed
Ream 2015 {published data only}
-
- Ream E, Gargaro G, Barsevick A, Richardson A. Management of cancer-related fatigue during chemotherapy through telephone motivational interviewing: modeling and randomized exploratory trial. Patient Education and Counseling 2015;98:199-206. - PubMed
Reese 2014 {published data only}
Reese 2018 {published data only}
Sherwood 2005 {published data only}
Sikorskii 2007 {published data only}
Thomas 2012 {published data only}
-
- Thomas M, Elliott J, Rao S, Fahey K, Paul S, Miaskowski C. A randomized, clinical trial of education or motivational-interviewing–based coaching compared to usual care to improve cancer pain management. Oncology Nursing Forum 2012;39(1):39-49. - PubMed
Traeger 2015 {published data only}
-
- Traeger L, Mcdonnell T, McCarty C, Greer J, El-Jawahri A, Temel J. Nursing intervention to enhance outpatient chemotherapy symptom management: patient reported outcomes of a randomized controlled trial. Cancer 2015;1:3905-13. - PubMed
Watson 2017 {published data only}
-
- Watson M, White C, Lynch A, Mohammed K. Telephone‐delivered individual cognitive behavioural therapy for cancer patients: an equivalence randomised trial. Psycho-oncology 2017;26:301-8. - PubMed
Yates 2005 {published data only}
-
- Yates P, Aranda S, Hargraves M, Mirolo B, Clavarino A, McLachlan S, et al. Randomized controlled trial of an educational intervention for managing fatigue in women receiving adjuvant chemotherapy for early-stage breast cancer. Journal of Clinical Oncology 2005;23(25):6027-36. - PubMed
References to studies excluded from this review
Aranda 2006 {published data only}
Ashing‐Giwa 2008 {published data only}
-
- Ashing-GiwaK T. Enhancing physical well-being and overall quality of life among underserved Latina-American cervical cancer survivors: feasibility study. Journal of Cancer Survivorship 2008;2:215–23. - PubMed
Bakitas 2009 {published data only}
-
- Bakitas M, Hegel MT, Balan S, Barnett KN, Brokaw FC, Byock IR, et al. The project ENABLE II randomized controlled trial to improve palliative care for rural patients with advanced cancer: baseline findings, methodological challenges and solutions. Palliative & Supportive Care 2009;7:75-86. - PMC - PubMed
Beaver 2006 {published data only}
-
- Beaver K, Twomey M, Whitham G, Foy S, Luke KA. Meeting the information needs of women with breast cancer: piloting a nurse-led intervention. European Journal of Oncology Nursing 2006;10:378–90. - PubMed
Beaver 2009 {published data only}
Beney 2002 {published data only}
-
- Beney J, Devine EB, Chow V, Ignoffo RJ, Mitsunaga L, Shahkarami M, et al. Effect of telephone follow-up on the physical well-being dimension of quality of life in patients with cancer. Pharmacotherapy 2002;22(10):1301–11. - PubMed
Bohnenkamp 2004 {published data only}
-
- Bohnekamp SK, McDonald P, Lopez AM, Krupinski E, Blackett A. Traditional versus telenursing outpatient management of patients with cancer with new ostomies. Oncology Nursing Forum 2004;31(5):1005-10. - PubMed
Budin 2008 {published data only}
-
- Budin WC, Hoskins CN, Haber J, Sherman DW, Maislin G, Cater JR, et al. Education, counseling, and adjustment among patients and partners: a randomized clinical trial. Nursing Research 2008;57(3):199-213. - PubMed
Campbell 2007 {published data only}
-
- Campbell LC, Keefe FJ, Scipio C, McKee DC, Edwards CL, Herman SH, et al. Facilitating research participation and improving quality of life for African American prostate cancer survivors and their intimate partners. American Cancer Society 2007;109(2):414-24. - PubMed
Cheville 2013 {published data only}
-
- Cheville A, Kollasch J, Vandenberg J, Shen T, Grothey A, Gamble G, et al. A home-based exercise program to improve function, fatigue, and sleep quality in patients with stage IV lung and colorectal cancer: a randomized controlled trial. Journal of Pain and Symptom Management 2013;45(5):811-21. - PMC - PubMed
Coleman 2005 {published data only}
-
- Coleman EA, Tulman L, Samarel N, Wilmoth MC, Rickel L, Rickel M, et al. The effect of telephone social support and education on adaptation to breast cancer during the year following diagnosis. Oncology Nursing Forum 2005;32(4):822-9. - PubMed
Collie 2006 {published data only}
-
- Collie K, Kreshka MA, Ferrier S, Parsons R, Graddy K, Avram S, et al. Videoconferencing for delivery of breast cancer support groups to women living in rural communities: a pilot study. Psycho-oncology 2007;16:778–82. - PubMed
Craddock 1999 {published data only}
-
- Craddock R, Adams P, Usui W, Mitchell L. An intervention to increase use and effectiveness of self-care measures for breast cancer chemotherapy patients. Cancer Nursing 1999;22(4):312-9. - PubMed
Dalton 2004 {published data only}
-
- Dalton JA, Keefe FJ, Carlson J, Youngblood R . Tailoring cognitive-behavioral treatment for cancer pain. Pain Management Nursing 2004;5(1):3-18. - PubMed
De Wit 1997 {published data only}
-
- De Wit R, Van Dam F, Zandbelt L, Van Buuren A, Van Der Heijden K, Leenhouts G, et al. A pain education program for chronic cancer pain patients: follow-up results from a randomized controlled trial. Pain 1997;73:55-69. - PubMed
DuHamel 2015 {published data only}
Given 2008 {published data only}
Haddad 2003 {published data only}
-
- Haddad P, Wilson P, Wong R, Williams D, Sharma N, Soban F, et al. The success of data collection in the palliative setting - telephone or clinic follow-up? Supportive Care in Cancer 2003;11:555-9. - PubMed
Hagiopan 1990 {published data only}
-
- Hagopian GA, Rubenstein JH. Effects of telephone call interventions on patients' well-being in a radiation therapy department. Cancer Nursing 1990;13(6):339-44. - PubMed
Halbert 2004 {published data only}
-
- Halbert CH, Wenzel L, Lerman C, Peshkin BN, Narod S, Marcus A, et al. Predictors of participation in psychosocial telephone counseling following genetic testing for BRCA1and BRCA2 mutations. Cancer Epidemiology, Biomarkers & Prevention 2004;13(5):875-81. - PubMed
Hanks 2002 {published data only}
Harrison 2011 {published data only}
-
- Harrison JD, Young JM, Soloman MJ, Butow PN, Secomb R, Masya L. Randomized pilot evaluation of the supportive care intervention “CONNECT” for people following surgery for colorectal cancer. Diseases of the Colon & Rectum 2011;54(5):622-31. - PubMed
Hawkes 2009 {published data only}
-
- Hawkes AL, Gollschewski S, Lynch BM, Chambers S. A telephone-delivered lifestyle intervention for colorectal cancer survivors ‘CanChange’: a pilot study. Psycho-oncology 2009;18:449–55. - PubMed
Hawkins 2010 {published data only}
Hayes 2012 {published data only}
-
- Hayes SC, Rye S, Disipio T, Yates P, Bashford J, Pyke C, et al. Exercise for health: a randomized, controlled trial evaluating the impact of a pragmatic, translational exercise intervention on the quality of life, function and treatment related side-effects following breast cancer. Breast Cancer Research and Treatment 2013;137:175-86. - PubMed
Kearney 2009 {published data only}
-
- Kearney N, McCann L, Norrie J, Taylor L, Gray P, McGee-Lennon M, et al. Evaluation of a mobile phone-based, advanced symptom management system (ASyMS©) in the management of chemotherapy-related toxicity. Supportive Care in Cancer 2009;17:437-44. - PubMed
Kimman 2010 {published data only}
-
- Kimman ML, Dirksen CD, Voogd AC, Falger P, Gijsen BCM, Thuring MT, et al. Nurse-led telephone follow-up and an educational group programme after breast cancer treatment: results of a 2x2 randomised controlled trial. European Journal of Cancer 2011;47:1027-36. - PubMed
Koller 2013 {published data only}
-
- Koller A, Miaskowski C, De Geest S, Opitz O, Spichiger E. Results of a randomized controlled pilot study of a self-management intervention for cancer pain. European Journal of Oncology Nursing 2013;17:284-91. - PubMed
Kornblinth 2006 {published data only}
-
- Kornblith AB, Dowell JM, Herndon JE, Engelman BJ, Bauer-Wu S, Small EJ, et al. Telephone monitoring of distress in patients aged 65 years or older with advanced stage cancer. A cancer and leukemia group B study. Cancer 2006;107:2706–14. - PubMed
Marcus 2010 {published data only}
McCorkle 2009 {published data only}
Meneses 2009 {published data only}
Nguyen 2018 {published data only}
-
- Nguyen L, Alexander K, Yates P. Psychoeducational Intervention for Symptom Management of Fatigue, Pain, and Sleep Disturbance Cluster Among Cancer Patients: A Pilot Quasi-Experimental Study. Journal of Pain and Symptom Management 2018;55(6):1459-72. - PubMed
Park 2012 {published data only}
-
- Park JH, Bae SH, Jung YS, KIM KS. Quality of life and symptom experience in breast cancer survivors after participating in a psychoeducational support program. A pilot study. Cancer Nursing 2012;35(1):E34-41. - PubMed
Rustoen 2014 {published data only}
-
- Rustoen T, Valeberg B, Kolstad E, WIist E, Paul S, Miaskowski C. A randomized clinical trial of the efficacy of a self-care intervention to improve cancer pain management. Cancer Nursing 2014;37(1):34-43. - PubMed
Salonen 2009 {published data only}
-
- Salonen P, Tarkka MT, Kellokumpu-Lehtinen PL, Aastedt-Kurki P, Luukkaala T, Kaunonen M. Telephone intervention and quality of life in patients with breast cancer. Cancer Nursing 2009;32(3):177-90. - PubMed
Sandgren 2000 {published data only}
-
- Sandgren AK, McCaul KD, King B, O'Donnell S, Foreman G. Telephone therapy for patients with breast cancer. Oncology Nursing Forum 2000;27(4):683-8. - PubMed
Sandgren 2003 {published data only}
-
- Sandgren AK, McCaul KD. Short-term effects of telephone therapy for breast cancer patient. Health Psychology 2003;22(3):310–15. - PubMed
Sandgren 2007 {published data only}
-
- Sandgren AK, McCaul KD. Long-term telephone therapy outcomes for breast cancer patients. Psycho-oncology 2007;16:38-47. - PubMed
Santacroce 2010 {published data only}
-
- Santacroce SJ, Asmus K, Kadan-Lottick N, Grey M. Feasibility and preliminary outcomes from a pilot study of coping skills training for adolescent-young adult survivors of childhood cancer and their parents. Journal of Pediatric Oncology Nursing 2010;27(1):10-20. - PubMed
Sikorskii 2009 {published data only}
Sikorskii 2009b {published data only}
Spoelstra 2013 {published data only}
-
- Spoelstra S, Given B, Given C, Grant M, Sikorskii A, You M, et al. An intervention to improve adherence and management of symptoms for patients prescribed oral chemotherapy agents. Cancer Nursing 2013;36(1):18-28. - PubMed
Williams 2004 {published data only}
-
- Williams SA, Schreier AM. The effect of education in managing side effects in women receiving chemotherapy for treatment of breast cancer. Oncology Nursing Forum 2004;31(1):E16-23. - PubMed
Winger 2018 {published data only}
-
- Winger J, Rand K, Hanna N, Jalal S, Einhorn L, Birdas T, et al. Coping skills practice and symptom change: a secondary analysis of a pilot telephone symptom management intervention for lung cancer patients and their family caregivers. Journal of Pain and Symptom Management 2018;55:1341-9. - PMC - PubMed
Additional references
Abrams 2005
-
- Abrams K, Gillies C, Lambert P. Meta-analysis of heterogeneously reported trials assessing change from baseline. Statistics in Medicine 2005;24:3823-44. - PubMed
Ahlberg 2003
-
- Ahlberg K, Ekman T, Gaston-Johansson F, Mock V. Assessment and management of cancer-related fatigue in adults. Lancet 2003;362:640-50. - PubMed
Barsevick 2002
-
- Barsevick A, Sweeney C, Haney E, Chung E. A systematic qualitative analysis of psychoeducational interventions for depression in patients with cancer. Oncology Nursing Forum 2002;1:73-84. - PubMed
Chen 2018
-
- Chen Y, Bing-Sheng G, Li Z, Li X. Effect of telehealth intervention on breast cancer patients’ quality of life and psychological outcomes: a meta-analysis. Journal of Telemedicine and Telecare 2018;24(3):157-67. - PubMed
Cheville 2010
Cleeland 2009
-
- Cleeland C. Symptom burden: multiple symptoms and their impact as patient-reported outcomes. Journal of the National Cancer Institute Monographs 2009;37:16-21. - PubMed
Cox 2003
-
- Cox K, Wilson E. Follow-up for people with cancer: nurse-led services and telephone interventions. Journal of Advanced Nursing 2003;43:51-61. - PubMed
DerSimonian 1986
-
- DerSimonian R, Laird N. Meta-analysis in clinical trials. Controlled Clinical Trials 1986;7:177-88. - PubMed
Dickinson 2014
Dieng 2016
-
- Dieng M, Butow P, Costa D, Morton R, Menzies S, Mireskandari S. Psychoeducational intervention to reduce fear of cancer recurrence in people at high risk of developing another primary melanoma: results of a randomized controlled trial. Journal of Clinical Oncology 2016;34:4405-14. - PubMed
Dodd 2000
-
- Dodd M, Miaskowski C. The PRO-SELF program: a self-care intervention program for patients receiving cancer treatment. Seminars in Oncology Nursing 2000;16:300-8. - PubMed
Dodd 2001
-
- Dodd M, Miaskowski C, Paul S. Symptom clusters and their effect on the functional status of patients with cancer. Oncology Nursing Forum 2001;28:465-70. - PubMed
Follmann 1992
-
- Follmann D, Elliott P, Suh I, Cutler J. Variance imputation for overviews of clinical trials with continuous response. Journal of Clinical Epidemiology 1992;45:769-73. - PubMed
Freeman 2015
Galway 2012
Gil 2006
-
- Gil K, Mishel M, Belyea M, Germino B, Porter L, Clayton M. Benefits of the uncertainty management intervention for African American and White older breast cancer survivors: 20-month outcomes. International Journal of Behavioural Medicine 2006;13(4):286-94. - PubMed
Glover 1995
-
- Glover J, Miaskowski C, Dibble S, Dodd M. Mood states of oncology outpatients: does pain make a difference? Journal of Pain and Symptom Management 1995;10:120-8. - PubMed
Gotay 1998
-
- Gotay C, Bottomley A. Providing psycho-social support by telephone: what is the potential for cancer patients? European Journal of Cancer Care 1998;7:225-31. - PubMed
Harrington 2010
-
- Harrington C, Hansen J, Moskowitz M, Todd B, Feuerstein M. It's not over when it's over: long-term symptoms in cancer survivors - a systematic review. International Journal of Psychiatry in Medicine 2010;40(2):163-81. - PubMed
Higgins 2003
Kim 2004
-
- Kim J, Dodd M, West C, Paul S, Facione N, Schumacher K, et al. The PRO-SELF pain control program improves patients' knowledge of cancer pain management. Oncology Nursing Forum 2004;31:1137-43. - PubMed
Kim 2009
Kim 2012
-
- Kim H, Barsevick A, Fang C, Miaskowski C. Common biological pathways underlying the psychoneurological symptom cluster in cancer patients. Cancer Nursing 2012;35(6):E1-20. - PubMed
Laugsand 2011
Lins 2014
McPherson 2014
Reese 2002
-
- Reese R, Conoley C, Brossart D. Effects of telephone counselling: a field-based investigation. Journal of Counselling Psychology 2002;49:233-42.
RevMan 2014 [Computer program]
-
- The Nordic Cochrane Centre, The Cochrane Collaboration, Copenhagen Review Manager (RevMan). Version 5.3. The Nordic Cochrane Centre, The Cochrane Collaboration, Copenhagen, 2014.
Scura 2004
-
- Scura K, Budin W, Garging E. Telephone social support and education for adaptation to prostate cancer: a pilot study. Oncology Nursing Forum 2004;31:335-8. - PubMed
Steel 2016
Van Lancker 2014
-
- Van Lancker A, Velghe A, Van Hecke A, Verbrugghe M, Van Den Noortgate N, Grypdonck M, et al. Prevalence of symptoms in older cancer patients receiving palliative care: a systematic review and meta-analysis. Journal of Pain and Symptom Management 2014;47(1):90-104. - PubMed
Walsh 2000
-
- Walsh D, Donnelly S, Rybicki L. The symptoms of advanced cancer: relationship to age, gender, and performance status in 1,000 patients. Supportive Care in Cancer 2000;8(3):175-9. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Research Materials

