Review of the evidence regarding the use of antenatal multiple micronutrient supplementation in low- and middle-income countries
- PMID: 31134643
- PMCID: PMC6852202
- DOI: 10.1111/nyas.14121
Review of the evidence regarding the use of antenatal multiple micronutrient supplementation in low- and middle-income countries
Abstract
Inadequate micronutrient intakes are relatively common in low- and middle-income countries (LMICs), especially among pregnant women, who have increased micronutrient requirements. This can lead to an increase in adverse pregnancy and birth outcomes. This review presents the conclusions of a task force that set out to assess the prevalence of inadequate micronutrient intakes and adverse birth outcomes in LMICs; the data from trials comparing multiple micronutrient supplements (MMS) that contain iron and folic acid (IFA) with IFA supplements alone; the risks of reaching the upper intake levels with MMS; and the cost-effectiveness of MMS compared with IFA. Recent meta-analyses demonstrate that MMS can reduce the risks of preterm birth, low birth weight, and small for gestational age in comparison with IFA alone. An individual-participant data meta-analysis also revealed even greater benefits for anemic and underweight women and female infants. Importantly, there was no increased risk of harm for the pregnant women or their infants with MMS. These data suggest that countries with inadequate micronutrient intakes should consider supplementing pregnant women with MMS as a cost-effective method to reduce the risk of adverse birth outcomes.
Keywords: LMICs; micronutrient; pregnancy; supplements.
© 2019 The Authors. Annals of the New York Academy of Sciences published by Wiley Periodicals, Inc. on behalf of New York Academy of Sciences.
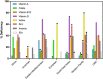
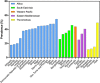
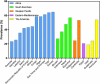
Figures

Similar articles
-
Modifiers of the effect of maternal multiple micronutrient supplementation on stillbirth, birth outcomes, and infant mortality: a meta-analysis of individual patient data from 17 randomised trials in low-income and middle-income countries.Lancet Glob Health. 2017 Nov;5(11):e1090-e1100. doi: 10.1016/S2214-109X(17)30371-6. Lancet Glob Health. 2017. PMID: 29025632
-
Antenatal multiple micronutrient supplements versus iron-folic acid supplements and birth outcomes: Analysis by gestational age assessment method.Matern Child Nutr. 2023 Jul;19(3):e13509. doi: 10.1111/mcn.13509. Epub 2023 Mar 31. Matern Child Nutr. 2023. PMID: 37002655 Free PMC article.
-
Multiple Micronutrient Supplements Are More Cost-effective Than Iron and Folic Acid: Modeling Results from 3 High-Burden Asian Countries.J Nutr. 2019 Jul 1;149(7):1222-1229. doi: 10.1093/jn/nxz052. J Nutr. 2019. PMID: 31131412
-
Multiple-micronutrient supplementation for women during pregnancy.Cochrane Database Syst Rev. 2017 Apr 13;4(4):CD004905. doi: 10.1002/14651858.CD004905.pub5. Cochrane Database Syst Rev. 2017. Update in: Cochrane Database Syst Rev. 2019 Mar 14;3:CD004905. doi: 10.1002/14651858.CD004905.pub6. PMID: 28407219 Free PMC article. Updated. Review.
-
Multiple-micronutrient supplementation for women during pregnancy.Cochrane Database Syst Rev. 2015 Nov 1;2015(11):CD004905. doi: 10.1002/14651858.CD004905.pub4. Cochrane Database Syst Rev. 2015. Update in: Cochrane Database Syst Rev. 2017 Apr 13;4:CD004905. doi: 10.1002/14651858.CD004905.pub5. PMID: 26522344 Free PMC article. Updated. Review.
Cited by
-
Making the health system work for the delivery of nutrition interventions.Matern Child Nutr. 2021 Jan;17(1):e13056. doi: 10.1111/mcn.13056. Epub 2020 Jul 20. Matern Child Nutr. 2021. PMID: 32691489 Free PMC article.
-
Zinc Supplementation Initiated Prior to or During Pregnancy Modestly Impacted Maternal Status and High Prevalence of Hypozincemia in Pregnancy and Lactation: The Women First Preconception Maternal Nutrition Trial.J Nutr. 2024 Jun;154(6):1917-1926. doi: 10.1016/j.tjnut.2024.04.018. Epub 2024 Apr 16. J Nutr. 2024. PMID: 38621624 Free PMC article. Clinical Trial.
-
Multiple micronutrient supplements versus iron-folic acid supplements and maternal anemia outcomes: an iron dose analysis.Ann N Y Acad Sci. 2022 Jun;1512(1):114-125. doi: 10.1111/nyas.14756. Epub 2022 Feb 25. Ann N Y Acad Sci. 2022. PMID: 35218047 Free PMC article.
-
Exploring Perceptions and Needs of Mobile Health Interventions for Nutrition, Anemia, and Preeclampsia among Pregnant Women in Underprivileged Indian Communities: A Cross-Sectional Survey.Nutrients. 2023 Aug 24;15(17):3699. doi: 10.3390/nu15173699. Nutrients. 2023. PMID: 37686731 Free PMC article.
-
Global Trends and Future Prospects of Child Nutrition: A Bibliometric Analysis of Highly Cited Papers.Front Pediatr. 2021 Sep 9;9:633525. doi: 10.3389/fped.2021.633525. eCollection 2021. Front Pediatr. 2021. PMID: 34568235 Free PMC article. Review.
References
-
- United States Department of Agriculture . 2019. Pregnancy. Accessed April 24, 2019. https://www.nutrition.gov/subject/life-stages/women/pregnancy.
-
- Smith, E.R. , Shankar A.H., Wu L.S.‐F., et al 2017. Modifiers of the effect of maternal multiple micronutrient supplementation on stillbirth, birth outcomes, and infant mortality: a meta‐analysis of individual patient data from 17 randomised trials in low‐income and middle‐income countries. Lancet Glob. Health 5: e1090–e1100. - PubMed
-
- World Health Organization . 2016. World Health Organization recommendations on antenatal care for a positive pregnancy experience. Geneva: WHO. - PubMed

