UMOD gene mutations in Chinese patients with autosomal dominant tubulointerstitial kidney disease: a pediatric case report and literature review
- PMID: 31068150
- PMCID: PMC6505284
- DOI: 10.1186/s12887-019-1522-7
UMOD gene mutations in Chinese patients with autosomal dominant tubulointerstitial kidney disease: a pediatric case report and literature review
Abstract
Background: Autosomal dominant tubulointerstitial kidney disease (ADTKD) caused by UMOD gene mutation (ADTKD-UMOD) is rare in children, characterized by hyperuricemia, gout, and progressive chronic kidney disease. It usually leads to end-stage renal failure at fiftieth decades. Here, we report a 3-year-old Chinese boy in an ADTKD family caused by a novel UMOD gene mutation.
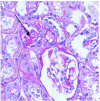
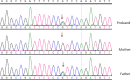
Case presentation: A 3-year-old boy was admitted to our hospital because of persistent hematuria. Urinalysis showed BLD 2+ without proteinuria. The serum levels of uric acid, creatinine and electrolytes were normal. No renal cyst or calculus was found by ultrasonography. Renal biopsy was performed and focal and segmental glomerulosclerosis was found in 4 glomeruli among 35 glomeruli examined. His father was found with end-stage renal disease (ESRD) at the age of 29, and renal ultrasound showed several cysts in both kidneys. A novel heterozygous mutation (c.1648G > A,p.V550I) in exon 8 of UMOD gene was identified by whole exome sequencing in the family. SCBC Genome Browser alignment showed that V550 were highly conserved in uromodulin among different species. Software predicted that the mutation is suspected to be harmful. By literature review, there are 12 mutations of UMOD gene in 14 Chinese families including only one pediatric case(a 16-year-old girl).
Conclusions: A novel heterozygous mutation (c.1648G > A,p.V550I) in exon 8 of UMOD gene was found in in a Chinese child case with ADTKD-UMOD, which extends our understanding of UMOD gene mutation spectrum and phenotype of ADTKD-UMOD in children.
Keywords: Autosomal dominant tubulointerstitial kidney disease; ESRD; Gout; Hyperuricemia; UMOD gene mutation.
Conflict of interest statement
Ethics approval and consent to participate
The study was approved by The Human Ethics Committees of the Tongji Hospital, Tongji Medical College, Huazhong University of Science and Technology(TJ-IRB20171113).
Consent for publication
We obtained written informed consent for the publication of this case report, including any identifiable data and images from the parents of the patient.
Competing interests
The authors declare that they have no competing interests.
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Figures


Similar articles
-
A novel uromodulin mutation in autosomal dominant tubulointerstitial kidney disease: a pedigree-based study and literature review.Ren Fail. 2018 Nov;40(1):146-151. doi: 10.1080/0886022X.2018.1450757. Ren Fail. 2018. PMID: 29569962 Free PMC article. Review.
-
Autosomal Dominant Tubulointerstitial Kidney Disease: Clinical Presentation of Patients With ADTKD-UMOD and ADTKD-MUC1.Am J Kidney Dis. 2018 Sep;72(3):411-418. doi: 10.1053/j.ajkd.2018.03.019. Epub 2018 May 18. Am J Kidney Dis. 2018. PMID: 29784615
-
Autosomal Dominant Tubulointerstitial Kidney Disease Due to UMOD Mutation: A Two-Case Report and Literature Review.Nephron. 2019;143(4):282-287. doi: 10.1159/000502146. Epub 2019 Aug 16. Nephron. 2019. PMID: 31422399 Review.
-
A novel likely pathogenic variant in the UMOD gene in a family with autosomal dominant tubulointerstitial kidney disease: a case report.BMC Nephrol. 2020 Aug 26;21(1):368. doi: 10.1186/s12882-020-02022-1. BMC Nephrol. 2020. PMID: 32847529 Free PMC article.
-
Autosomal dominant tubulointerstitial kidney disease-UMOD is the most frequent non polycystic genetic kidney disease.BMC Nephrol. 2018 Oct 30;19(1):301. doi: 10.1186/s12882-018-1107-y. BMC Nephrol. 2018. PMID: 30376835 Free PMC article.
Cited by
-
Susceptibility genes of hyperuricemia and gout.Hereditas. 2022 Aug 4;159(1):30. doi: 10.1186/s41065-022-00243-y. Hereditas. 2022. PMID: 35922835 Free PMC article. Review.
-
Upregulation of C/EBP Homologous Protein induced by ER Stress Mediates Epithelial to Myofibroblast Transformation in ADTKD-UMOD.Int J Med Sci. 2022 Jan 24;19(2):364-376. doi: 10.7150/ijms.65036. eCollection 2022. Int J Med Sci. 2022. PMID: 35165522 Free PMC article.
-
Autosomal dominant tubulointerstitial kidney disease genotype and phenotype correlation in a Chinese cohort.Sci Rep. 2021 Feb 11;11(1):3615. doi: 10.1038/s41598-020-79331-w. Sci Rep. 2021. PMID: 33574344 Free PMC article.
References
-
- Eckardt KU, Alper SL, Antignac C, Bleyer AJ, Chauveau D, Dahan K, Deltas C, Hosking A, Kmoch S, Rampoldi L, Wiesener M, Wolf MT, Devuyst O. Autosomal dominant tubulointerstitial kidney disease: diagnosis, classification, and management--a KDIGO consensus report. Kidney Int. 2015;88:676–683. doi: 10.1038/ki.2015.28. - DOI - PubMed
-
- Hart TC, Gorry MC, Hart PS, Woodard AS, Shihahi Z, Sandhu J, Shirts B, Xu L, Zhu H, Barmada MM, Bleyer AJ. Mutations of the UMOD gene are responsible for medullary cystic kidney disease 2 and familial juvenile hyperuricaemic nephropathy. J Med Genet. 2002;39:882–892. doi: 10.1136/jmg.39.12.882. - DOI - PMC - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Miscellaneous

