PR interval prolongation in coronary patients or risk equivalent: excess risk of ischemic stroke and vascular pathophysiological insights
- PMID: 28836952
- PMCID: PMC5571504
- DOI: 10.1186/s12872-017-0667-2
PR interval prolongation in coronary patients or risk equivalent: excess risk of ischemic stroke and vascular pathophysiological insights
Abstract
Background: Whether PR prolongation independently predicts new-onset ischemic events of myocardial infarction and stroke was unclear. Underlying pathophysiological mechanisms of PR prolongation leading to adverse cardiovascular events were poorly understood. We investigated the role of PR prolongation in pathophysiologically-related adverse cardiovascular events and underlying mechanisms.
Methods: We prospectively investigated 597 high-risk cardiovascular outpatients (mean age 66 ± 11 yrs.; male 67%; coronary disease 55%, stroke 22%, diabetes 52%) for new-onset ischemic stroke, myocardial infarction (MI), congestive heart failure (CHF), and cardiovascular death. Vascular phenotype was determined by carotid intima-media thickness (IMT).
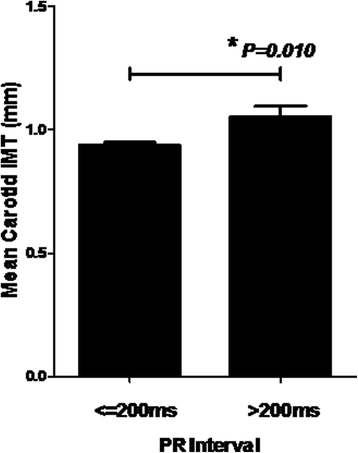
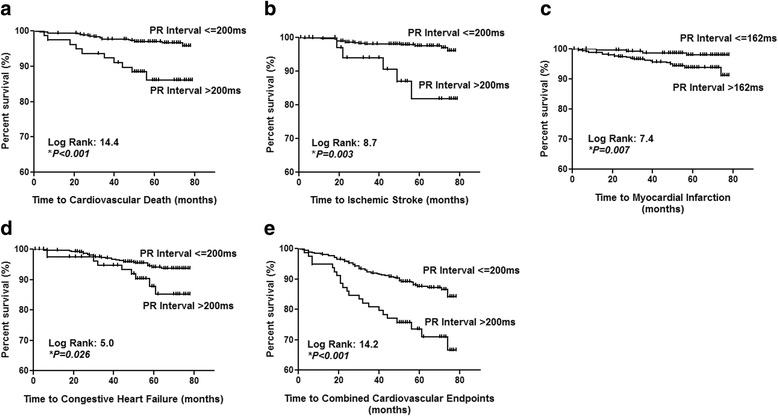
Results: PR prolongation >200 ms was present in 79 patients (13%) at baseline. PR prolongation >200 ms was associated with significantly higher mean carotid IMT (1.05 ± 0.37 mm vs 0.94 ± 0.28 mm, P = 0.010). After mean study period of 63 ± 11 months, increased PR interval significantly predicted new-onset ischemic stroke (P = 0.006), CHF (P = 0.040), cardiovascular death (P < 0.001), and combined cardiovascular endpoints (P < 0.001) at cut-off >200 ms. Using multivariable Cox regression, PR prolongation >200 ms independently predicted new-onset ischemic stroke (HR 8.6, 95% CI: 1.9-37.8, P = 0.005), cardiovascular death (HR 14.1, 95% CI: 3.8-51.4, P < 0.001) and combined cardiovascular endpoints (HR 2.4, 95% CI: 1.30-4.43, P = 0.005). PR interval predicts new-onset MI at the exploratory cut-off >162 ms (C-statistic 0.70, P = 0.001; HR: 8.0, 95% CI: 1.65-38.85, P = 0.010).
Conclusions: PR prolongation strongly predicts new-onset ischemic stroke, MI, cardiovascular death, and combined cardiovascular endpoint including CHF in coronary patients or risk equivalent. Adverse vascular function may implicate an intermediate pathophysiological phenotype or mediating mechanism.
Keywords: Cardiovascular death; Carotid intima-media thickness; Ischemic stroke; Myocardial infarction; PR interval prolongation; Pathophysiological mechanism; Vascular function.
Conflict of interest statement
Ethics approval and consent to participate
We declare that all patients completed written informed consent and the study was adherent to the Declaration of Helsinki and approved by the Ethics Committee, Hospital Authority (Hong Kong West)/ University of Hong Kong.
Consent for publication
We declare that all patients gave informed consent to the research participation and its publication.
Competing interests
The authors declare that they have no competing interests.
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Figures
Similar articles
-
The CHADS2 and CHA2DS2-VASc scores predict adverse vascular function, ischemic stroke and cardiovascular death in high-risk patients without atrial fibrillation: role of incorporating PR prolongation.Atherosclerosis. 2014 Dec;237(2):504-13. doi: 10.1016/j.atherosclerosis.2014.08.026. Epub 2014 Aug 30. Atherosclerosis. 2014. PMID: 25463082
-
Cardiovascular outcomes among elderly patients with heart failure and coronary artery disease and without atrial fibrillation: a retrospective cohort study.BMC Cardiovasc Disord. 2019 Jan 15;19(1):19. doi: 10.1186/s12872-018-0991-1. BMC Cardiovasc Disord. 2019. PMID: 30646855 Free PMC article.
-
Noninvasive detection of increased carotid artery temperature in patients with coronary artery disease predicts major cardiovascular events at one year: Results from a prospective multicenter study.Atherosclerosis. 2017 Jul;262:25-30. doi: 10.1016/j.atherosclerosis.2017.04.019. Epub 2017 Apr 23. Atherosclerosis. 2017. PMID: 28482222
-
Risk of myocardial infarction and vascular death after transient ischemic attack and ischemic stroke: a systematic review and meta-analysis.Stroke. 2005 Dec;36(12):2748-55. doi: 10.1161/01.STR.0000190118.02275.33. Epub 2005 Oct 27. Stroke. 2005. PMID: 16254218 Review.
-
Heart rate as a predictor of cardiovascular risk.Eur J Clin Invest. 2018 Mar;48(3). doi: 10.1111/eci.12892. Epub 2018 Feb 5. Eur J Clin Invest. 2018. PMID: 29355923 Review.
Cited by
-
Develop and Apply Electrocardiography-Based Risk Score to Identify Community-Based Elderly Individuals at High-Risk of Mortality.Front Cardiovasc Med. 2021 Oct 8;8:738061. doi: 10.3389/fcvm.2021.738061. eCollection 2021. Front Cardiovasc Med. 2021. PMID: 34692790 Free PMC article.
-
Prognostic significance of first-degree atrioventricular block in a large Asian population: a prospective cohort study.BMJ Open. 2022 Apr 4;12(4):e062005. doi: 10.1136/bmjopen-2022-062005. BMJ Open. 2022. PMID: 35379649 Free PMC article.
-
Osteogenic circulating endothelial progenitor cells are linked to electrocardiographic conduction abnormalities in rheumatic patients.Ann Noninvasive Electrocardiol. 2019 Sep;24(5):e12651. doi: 10.1111/anec.12651. Epub 2019 Apr 24. Ann Noninvasive Electrocardiol. 2019. PMID: 31017736 Free PMC article.
-
Epidemiology and Outcomes Associated with PR Prolongation.Card Electrophysiol Clin. 2021 Dec;13(4):661-669. doi: 10.1016/j.ccep.2021.06.007. Epub 2021 Sep 23. Card Electrophysiol Clin. 2021. PMID: 34689893 Free PMC article. Review.
-
PR interval prolongation and 1-year mortality among emergency department patients: a multicentre transnational cohort study.BMJ Open. 2021 Dec 14;11(12):e054238. doi: 10.1136/bmjopen-2021-054238. BMJ Open. 2021. PMID: 34907068 Free PMC article.
References
-
- Chan YH, Yiu KH, Lau KK, Yiu YF, Li SW, Lam TH, et al. The CHADS2 and CHA2DS2-VASc scores predict adverse vascular function, ischemic stroke and cardiovascular death in high-risk patients without atrial fibrillation: role of incorporating PR prolongation. Atherosclerosis. 2014;237(2):504–513. doi: 10.1016/j.atherosclerosis.2014.08.026. - DOI - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Research Materials

