MYH11 mutations result in a distinct vascular pathology driven by insulin-like growth factor 1 and angiotensin II
- PMID: 17666408
- PMCID: PMC2905218
- DOI: 10.1093/hmg/ddm201
MYH11 mutations result in a distinct vascular pathology driven by insulin-like growth factor 1 and angiotensin II
Erratum in
- Hum Mol Genet. 2008 Jan 1;17(1):158
Abstract
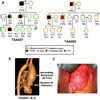
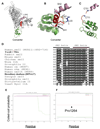
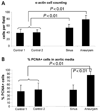
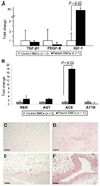
Non-syndromic thoracic aortic aneurysms and dissections (TAADs) are inherited in an autosomal dominant manner in approximately 20% of cases. Familial TAAD is genetically heterogeneous and four loci have been mapped for this disease to date, including a locus at 16p for TAAD associated with patent ductus arteriosus (PDA). The defective gene at the 16p locus has recently been identified as the smooth muscle cell (SMC)-specific myosin heavy chain gene (MYH11). On sequencing MYH11 in 93 families with TAAD alone and three families with TAAD/PDA, we identified novel mutations in two families with TAAD/PDA, but none in families with TAAD alone. Histopathological analysis of aortic sections from two individuals with MYH11 mutations revealed SMC disarray and focal hyperplasia of SMCs in the aortic media. SMC hyperplasia leading to significant lumen narrowing in some of the vessels of the adventitia was also observed. Insulin-like growth factor-1 (IGF-1) was upregulated in mutant aortas as well as explanted SMCs, but no increase in transforming growth factor-beta expression or downstream targets was observed. Enhanced expression of angiotensin-converting enzyme and markers of Angiotensin II (Ang II) vascular inflammation (macrophage inflammatory protein-1alpha and beta) were also found. These data suggest that MYH11 mutations are likely to be specific to the phenotype of TAAD/PDA and result in a distinct aortic and occlusive vascular pathology potentially driven by IGF-1 and Ang II.
Conflict of interest statement
Figures

Similar articles
-
Incomplete segregation of MYH11 variants with thoracic aortic aneurysms and dissections and patent ductus arteriosus.Eur J Hum Genet. 2013 May;21(5):487-93. doi: 10.1038/ejhg.2012.206. Epub 2012 Sep 12. Eur J Hum Genet. 2013. PMID: 22968129 Free PMC article.
-
Mutations in myosin heavy chain 11 cause a syndrome associating thoracic aortic aneurysm/aortic dissection and patent ductus arteriosus.Nat Genet. 2006 Mar;38(3):343-9. doi: 10.1038/ng1721. Epub 2006 Jan 29. Nat Genet. 2006. PMID: 16444274
-
Complex genotype-phenotype correlation of MYH11: new insights from monozygotic twins with highly variable expressivity and outcomes.BMC Med Genomics. 2024 May 21;17(1):135. doi: 10.1186/s12920-024-01908-5. BMC Med Genomics. 2024. PMID: 38773466 Free PMC article.
-
Genetic basis of thoracic aortic aneurysms and dissections: focus on smooth muscle cell contractile dysfunction.Annu Rev Genomics Hum Genet. 2008;9:283-302. doi: 10.1146/annurev.genom.8.080706.092303. Annu Rev Genomics Hum Genet. 2008. PMID: 18544034 Review.
-
[Familial thoracic aortic aneurysms and dissections can be divided into three different main categories].Lakartidningen. 2014 Feb 25;111(9-10):399-403. Lakartidningen. 2014. PMID: 24570135 Review. Swedish.
Cited by
-
Matrix-dependent perturbation of TGFβ signaling and disease.FEBS Lett. 2012 Jul 4;586(14):2003-15. doi: 10.1016/j.febslet.2012.05.027. Epub 2012 May 26. FEBS Lett. 2012. PMID: 22641039 Free PMC article. Review.
-
A deleterious MYH11 mutation causing familial thoracic aortic dissection.Hum Genome Var. 2015 Aug 6;2:15028. doi: 10.1038/hgv.2015.28. eCollection 2015. Hum Genome Var. 2015. PMID: 27081537 Free PMC article.
-
Latent TGFβ-binding proteins 1 and 3 protect the larval zebrafish outflow tract from aneurysmal dilatation.Dis Model Mech. 2022 Mar 1;15(3):dmm046979. doi: 10.1242/dmm.046979. Epub 2022 Mar 28. Dis Model Mech. 2022. PMID: 35098309 Free PMC article.
-
Elastic fibers and biomechanics of the aorta: Insights from mouse studies.Matrix Biol. 2020 Jan;85-86:160-172. doi: 10.1016/j.matbio.2019.03.001. Epub 2019 Mar 15. Matrix Biol. 2020. PMID: 30880160 Free PMC article. Review.
-
Endothelial cell-specific deficiency of Ang II type 1a receptors attenuates Ang II-induced ascending aortic aneurysms in LDL receptor-/- mice.Circ Res. 2011 Mar 4;108(5):574-81. doi: 10.1161/CIRCRESAHA.110.222844. Epub 2011 Jan 20. Circ Res. 2011. PMID: 21252156 Free PMC article.
References
-
- Lilienfeld DE, Gunderson PD, Sprafka JM, Vargas C. Epidemiology of aortic aneurysms: I. Mortality trends in the United States, 1951 to 1981. Arteriosclerosis. 1987;7:637–643. - PubMed
-
- Lindsay J., Jr Diagnosis and treatment of diseases of the aorta. Curr. Probl. Cardiol. 1997;22:485–542. - PubMed
-
- Biddinger A, Rocklin M, Coselli J, Milewicz DM. Familial thoracic aortic dilatations and dissections: a case control study. J. Vasc. Surg. 1997;25:506–511. - PubMed
-
- Coady MA, Davies RR, Roberts M, Goldstein LJ, Rogalski MJ, Rizzo JA, Hammond GL, Kopf GS, Elefteriades JA. Familial patterns of thoracic aortic aneurysms. Arch. Surg. 1999;134:361–367. - PubMed
-
- Loeys BL, Chen J, Neptune ER, Judge DP, Podowski M, Holm T, Meyers J, Leitch CC, Katsanis N, Sharifi N, et al. A syndrome of altered cardiovascular, craniofacial, neurocognitive and skeletal development caused by mutations in TGFBR1 or TGFBR2. Nat. Genet. 2005;37:275–281. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Molecular Biology Databases
Miscellaneous

