Dose-response relationship of serum ferritin and dietary iron intake with metabolic syndrome and non-alcoholic fatty liver disease incidence: a systematic review and meta-analysis
- PMID: 39410926
- PMCID: PMC11476413
- DOI: 10.3389/fnut.2024.1437681
Dose-response relationship of serum ferritin and dietary iron intake with metabolic syndrome and non-alcoholic fatty liver disease incidence: a systematic review and meta-analysis
Abstract
Aim: This study aims to assess the dose-response impact of iron load on systemic and hepatic metabolic disorders including metabolic syndrome (MetS) and non-alcoholic fatty liver disease (NAFLD).
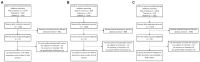
Methods: Serum ferritin (SF) and dietary iron intake were selected to represent the indicators of iron load in the general population. PubMed, EMBASE and Web of Science databases were searched for epidemiological studies assessing the impact of SF/dietary iron intake on MetS/NAFLD occurrence. All literature was published before September 1st, 2023 with no language restrictions.
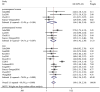
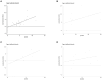
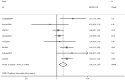
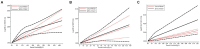
Results: Fifteen and 11 papers were collected with a focus on connections between SF and MetS/NAFLD, respectively. Eight papers focusing on dietary iron and MetS were included in the following meta-analysis. For the impact of SF on MetS, the pooled odds ratio (OR) of MetS was 1.88 (95% CI: 1.58-2.24) for the highest versus lowest SF categories. In males, the OR was 1.15 (95% CI: 1.10-1.21) per incremental increase in SF of 50 μg/L, while for females, each 50 μg/L increase in SF was associated with a 1.50-fold higher risk of MetS (95% CI: 1.15-1.94). For connections between SF and NAFLD, we found higher SF levels were observed in NAFLD patients compared to the control group [standardized mean difference (SMD) 0.71; 95% CI: 0.27-1.15], NASH patients against control group (SMD1.05; 95% CI:0.44-1.66), NASH patients against the NAFLD group (SMD 0.6; 95% CI: 0.31-1.00), each 50 μg/L increase in SF was associated with a 1.08-fold higher risk of NAFLD (95% CI: 1.07-1.10). For the impact of dietary iron on MetS, Pooled OR of MetS was 1.34 (95% CI: 1.10-1.63) for the highest versus lowest dietary iron categories.
Conclusion: Elevated SF levels is a linear relation between the incidence of MetS/NAFLD. In addition, there is a positive association between dietary iron intake and metabolic syndrome. The association between serum ferritin and metabolic syndrome may be confounded by body mass index and C-reactive protein levels.
Keywords: dietary iron; dose–response relationship; meta-analysis; metabolic syndrome; non-alcoholic fatty liver disease; serum ferritin.
Copyright © 2024 Yu, Que, Zhou and Liu.
Conflict of interest statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Figures


Similar articles
-
Association of Serum Bilirubin With Metabolic Syndrome and Non-Alcoholic Fatty Liver Disease: A Systematic Review and Meta-Analysis.Front Endocrinol (Lausanne). 2022 Jul 20;13:869579. doi: 10.3389/fendo.2022.869579. eCollection 2022. Front Endocrinol (Lausanne). 2022. PMID: 35937795 Free PMC article.
-
Complex impacts of gallstone disease on metabolic syndrome and nonalcoholic fatty liver disease.Front Endocrinol (Lausanne). 2022 Nov 23;13:1032557. doi: 10.3389/fendo.2022.1032557. eCollection 2022. Front Endocrinol (Lausanne). 2022. PMID: 36506064 Free PMC article.
-
Albuminuria Is Associated with Hepatic Iron Load in Patients with Non-Alcoholic Fatty Liver Disease and Metabolic Syndrome.J Clin Med. 2021 Jul 20;10(14):3187. doi: 10.3390/jcm10143187. J Clin Med. 2021. PMID: 34300354 Free PMC article.
-
Coffee and tea consumption in relation with non-alcoholic fatty liver and metabolic syndrome: A systematic review and meta-analysis of observational studies.Clin Nutr. 2016 Dec;35(6):1269-1281. doi: 10.1016/j.clnu.2016.03.012. Epub 2016 Mar 30. Clin Nutr. 2016. PMID: 27060021 Review.
-
Review article: coffee consumption, the metabolic syndrome and non-alcoholic fatty liver disease.Aliment Pharmacol Ther. 2013 Nov;38(9):1038-44. doi: 10.1111/apt.12489. Epub 2013 Sep 11. Aliment Pharmacol Ther. 2013. PMID: 24024834 Review.
References
Publication types
Grants and funding
LinkOut - more resources
Full Text Sources
Research Materials

