Current Landscape and Evolving Therapies for Primary Biliary Cholangitis
- PMID: 39329760
- PMCID: PMC11429758
- DOI: 10.3390/cells13181580
Current Landscape and Evolving Therapies for Primary Biliary Cholangitis
Abstract
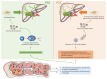
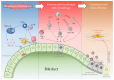
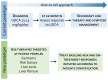
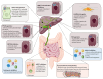
Primary Biliary Cholangitis (PBC) is a chronic autoimmune liver disorder characterized by progressive cholestatic that, if untreated, can progress to liver fibrosis, cirrhosis and liver decompensation requiring liver transplant. Although the pathogenesis of the disease is multifactorial, there is a consensus that individuals with a genetic predisposition develop the disease in the presence of specific environmental triggers. A dysbiosis of intestinal microbiota is increasingly considered among the potential pathogenic factors. Cholangiocytes, the epithelial cells lining the bile ducts, are the main target of a dysregulated immune response, and cholangiocytes senescence has been recognized as a driving mechanism, leading to impaired bile duct function, in disease progression. Bile acids are also recognized as playing an important role, both in disease development and therapy. Thus, while bile acid-based therapies, specifically ursodeoxycholic acid and obeticholic acid, have been the cornerstone of therapy in PBC, novel therapeutic approaches have been developed in recent years. In this review, we will examine published and ongoing clinical trials in PBC, including the recently approved peroxisome-proliferator-activated receptor (PPAR) agonist, elafibranor and seladelpar. These novel second-line therapies are expected to improve therapy in PBC and the development of personalized approaches.
Keywords: T cells; cholangiocytes; cholestasis; farnesoid-x-receptor (FXR); macrophages; peroxisome-proliferator-associated receptors (PPAR).
Conflict of interest statement
The authors declare no conflicts of interest.
Figures
Similar articles
-
PPAR-Mediated Bile Acid Glucuronidation: Therapeutic Targets for the Treatment of Cholestatic Liver Diseases.Cells. 2024 Aug 1;13(15):1296. doi: 10.3390/cells13151296. Cells. 2024. PMID: 39120326 Free PMC article. Review.
-
PPAR agonists for the treatment of cholestatic liver diseases: Over a decade of clinical progress.Hepatol Commun. 2024 Dec 20;9(1):e0612. doi: 10.1097/HC9.0000000000000612. eCollection 2025 Jan 1. Hepatol Commun. 2024. PMID: 39699308 Free PMC article. Review.
-
Primary biliary cholangitis: Personalizing second-line therapies.Hepatology. 2024 Nov 12. doi: 10.1097/HEP.0000000000001166. Online ahead of print. Hepatology. 2024. PMID: 39707635
-
Up-to-Date Snapshot of Current and Emerging Medical Therapies in Primary Biliary Cholangitis.J Pers Med. 2024 Nov 30;14(12):1133. doi: 10.3390/jpm14121133. J Pers Med. 2024. PMID: 39728045 Free PMC article. Review.
-
Depressing time: Waiting, melancholia, and the psychoanalytic practice of care.In: Kirtsoglou E, Simpson B, editors. The Time of Anthropology: Studies of Contemporary Chronopolitics. Abingdon: Routledge; 2020. Chapter 5. In: Kirtsoglou E, Simpson B, editors. The Time of Anthropology: Studies of Contemporary Chronopolitics. Abingdon: Routledge; 2020. Chapter 5. PMID: 36137063 Free Books & Documents. Review.
References
-
- Achufusi T.G.O., Safadi A.O., Mahabadi N. Ursodeoxycholic Acid. StatPearls Publishing; Treasure Island, FL, USA: 2024. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources

