e-income countries from a provider's perspective: a systematic review
- PMID: 32565428
- PMCID: PMC7309188
- DOI: 10.1136/bmjgh-2020-002371
e-income countries from a provider's perspective: a systematic review
Abstract
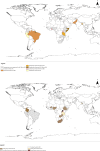
Introduction: Maternal health services are effective in reducing the morbidity and mortality associated with pregnancy and childbirth. We conducted a systematic review on costs of maternal health services in low-income and middle-income countries from the provider's perspective.
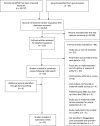
Methods: We searched multiple peer-reviewed databases (including African Journal Online, CINAHL Plus, EconLit, Popline, PubMed, Scopus and Web of Science) and grey literature for relevant articles published from year 2000. Articles meeting our inclusion criteria were selected with quality assessment done using relevant cost-focused criteria of the Consolidated Health Economic Evaluation Reporting Standards checklist. For comparability, disaggregated costs data were inflated to 2019 US$ equivalents. Costs and cost drivers were systematically compared. Where heterogeneity was observed, narrative synthesis was used to summarise findings.
Results: Twenty-two studies were included, with most studies costing vaginal and/or caesarean delivery (11 studies), antenatal care (ANC) (9) and postabortion care (PAC) (8). Postnatal care (PNC) has been least costed (2). Studies used different methods for data collection and analysis. Quality of peer-reviewed studies was assessed average to high while all grey literature studies were assessed as low quality. Following inflation, estimated provision cost per service varied (ANC (US$7.24-US$31.42); vaginal delivery (US$14.32-US$278.22); caesarean delivery (US$72.11-US$378.940; PAC (US$97.09-US$1299.21); family planning (FP) (US$0.82-US$5.27); PNC (US$5.04)). These ranges could be explained by intercountry variations, variations in provider type (public/private), facility type (primary/secondary) and care complexity (simple/complicated). Personnel cost was mostly reported as the major driver for provision of ANC, skilled birth attendance and FP. Economies of scale in service provision were reported.
Conclusion: There is a cost savings case for task-shifting and encouraging women to use lower level facilities for uncomplicated services. Going forward, consensus regarding cost component definitions and methodologies for costing maternal health services will significantly help to improve the usefulness of cost analyses in supporting policymaking towards achieving Universal Health Coverage.
Keywords: health economics; maternal health; systematic review.
© Author(s) (or their employer(s)) 2020. Re-use permitted under CC BY-NC. No commercial re-use. See rights and permissions. Published by BMJ.
Conflict of interest statement
Competing interests: None declared.
Figures
Similar articles
-
Cost of Utilising Maternal Health Services in Low- and Middle-Income Countries: A Systematic Review.Int J Health Policy Manag. 2021 Sep 1;10(9):564-577. doi: 10.34172/ijhpm.2020.104. Int J Health Policy Manag. 2021. PMID: 32610819 Free PMC article.
-
Cost of maternal health services in low and middle-income countries: protocol for a systematic review.BMJ Open. 2019 Aug 20;9(8):e027822. doi: 10.1136/bmjopen-2018-027822. BMJ Open. 2019. PMID: 31434768 Free PMC article.
-
Cost-effectiveness of strategies to improve the utilization and provision of maternal and newborn health care in low-income and lower-middle-income countries: a systematic review.BMC Pregnancy Childbirth. 2014 Jul 22;14:243. doi: 10.1186/1471-2393-14-243. BMC Pregnancy Childbirth. 2014. PMID: 25052536 Free PMC article. Review.
-
The impact of health insurance on maternal and reproductive health service utilization and financial protection in low- and lower middle-income countries: a systematic review of the evidence.BMC Health Serv Res. 2024 Apr 5;24(1):432. doi: 10.1186/s12913-024-10815-5. BMC Health Serv Res. 2024. PMID: 38580960 Free PMC article.
-
Factors influencing the free maternal health care policy under the national health insurance scheme's provision for skilled delivery services in Ghana: a narrative literature review.BMC Pregnancy Childbirth. 2023 Jun 14;23(1):439. doi: 10.1186/s12884-023-05730-2. BMC Pregnancy Childbirth. 2023. PMID: 37316790 Free PMC article. Review.
Cited by
-
The economic costs of orthopaedic services: a health system cost analysis of tertiary hospitals in a low-income country.Health Econ Rev. 2024 Feb 17;14(1):13. doi: 10.1186/s13561-024-00485-8. Health Econ Rev. 2024. PMID: 38367132 Free PMC article.
-
Exploring the association between multidimensional poverty and antenatal care utilization in two provinces of Papua New Guinea: a cross-sectional study.Int J Equity Health. 2024 Sep 2;23(1):176. doi: 10.1186/s12939-024-02241-0. Int J Equity Health. 2024. PMID: 39223487 Free PMC article.
-
Prevalence, influencing factors, and outcomes of emergency caesarean section in public hospitals situated in the urban state of Lagos, Nigeria.Afr Health Sci. 2023 Jun;23(2):640-651. doi: 10.4314/ahs.v23i2.74. Afr Health Sci. 2023. PMID: 38223597 Free PMC article.
-
Stakeholder perceptions and experiences from the implementation of the Gratuité user fee exemption policy in Burkina Faso: a qualitative study.Health Res Policy Syst. 2023 Jun 6;21(1):46. doi: 10.1186/s12961-023-01008-3. Health Res Policy Syst. 2023. PMID: 37280694 Free PMC article.
-
Equity in antenatal care visits among adolescent mothers: An analysis of 54 country levels trend and projection of coverage from 2000 to 2030.J Glob Health. 2022 Mar 19;12:04016. doi: 10.7189/jogh.12.04016. eCollection 2022. J Glob Health. 2022. PMID: 35356654 Free PMC article.
References
-
- United Nations Sustainable Development Goals: 17 goals to transform our world [Internet]. Sustainable Development Goals, 2016. Available: http://www.un.org/sustainabledevelopment/sustainable-development-goals/ [Accessed 20 Jun 2020].
-
- Alkema L, Chou D, Hogan D, et al. . Global, regional, and national levels and trends in maternal mortality between 1990 and 2015, with scenario-based projections to 2030: a systematic analysis by the un maternal mortality estimation Inter-Agency group. Lancet 2016;387:462–74. 10.1016/S0140-6736(15)00838-7 - DOI - PMC - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
