Association of Afamelanotide With Improved Outcomes in Patients With Erythropoietic Protoporphyria in Clinical Practice
- PMID: 32186677
- PMCID: PMC7081144
- DOI: 10.1001/jamadermatol.2020.0352
Association of Afamelanotide With Improved Outcomes in Patients With Erythropoietic Protoporphyria in Clinical Practice
Abstract
Importance: The effectiveness of afamelanotide treatment in patients with erythropoietic protoporphyria (EPP) in clinical practice who experience pain after light exposure that substantially impairs quality of life is unknown.
Objective: To evaluate the association of afamelanotide treatment with outcomes in patients with EPP in regular practice during longer-term follow-up.
Design, setting, and participants: This single-center, prospective postauthorization safety and efficacy cohort study was directed and approved by the European Medicines Agency. Data were collected from patients with EPP treated with afamelanotide at Erasmus MC between June 2016 and September 2018. Analysis began October 2018.
Main outcomes and measures: Time spent outside during treatment, number of phototoxic reactions, disease-specific quality of life, usage of protective clothing, and adverse events.
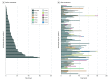
Results: A total of 117 patients with EPP (59 women [50.4%]; mean [SD] age, 43.0 [15.5] years) were treated with afamelanotide. Nearly all patients continued treatment (115 [98%]) with a median (interquartile range) follow-up of 2.0 (1.3-2.1) years. Compared with baseline, mean time spent outside during treatment increased significantly by an added 6.1 hours per week (95% CI, 3.62-8.67; P < .001). Mean quality of life score improved significantly by 14.01% (95% CI, 4.53%-23.50%; P < .001). Phototoxic reactions were less painful (β, -0.85; 95% CI, -1.43 to -0.26; P < .001), but there was no significant difference in number or duration of reactions. Minor self-limiting adverse events occurred, such as nausea, fatigue, and headache.
Conclusions and relevance: This cohort study found that afamelanotide treatment was associated with improved clinical outcomes and a good safety profile for patients with EPP. The treatment has clinically significant, sustained positive associations with quality of life, is associated with increased duration of sun exposure, and is associated with less severe phototoxic reactions.
Conflict of interest statement
Figures
Similar articles
-
Increased phototoxic burn tolerance time and quality of life in patients with erythropoietic protoporphyria treated with afamelanotide - a three years observational study.Orphanet J Rare Dis. 2020 Aug 18;15(1):213. doi: 10.1186/s13023-020-01505-6. Orphanet J Rare Dis. 2020. PMID: 32811524 Free PMC article.
-
Afamelanotide for prevention of phototoxicity in erythropoietic protoporphyria.Expert Rev Clin Pharmacol. 2021 Feb;14(2):151-160. doi: 10.1080/17512433.2021.1879638. Expert Rev Clin Pharmacol. 2021. PMID: 33507118 Review.
-
Long-term observational study of afamelanotide in 115 patients with erythropoietic protoporphyria.Br J Dermatol. 2015 Jun;172(6):1601-1612. doi: 10.1111/bjd.13598. Epub 2015 Apr 30. Br J Dermatol. 2015. PMID: 25494545 Clinical Trial.
-
Afamelanotide for Erythropoietic Protoporphyria.N Engl J Med. 2015 Jul 2;373(1):48-59. doi: 10.1056/NEJMoa1411481. N Engl J Med. 2015. PMID: 26132941 Free PMC article. Clinical Trial.
-
Afamelanotide: A Review in Erythropoietic Protoporphyria.Am J Clin Dermatol. 2016 Apr;17(2):179-85. doi: 10.1007/s40257-016-0184-6. Am J Clin Dermatol. 2016. PMID: 26979527 Review.
Cited by
-
Development and Content Validation of Novel Patient-Reported Outcome Measures to Assess Disease Severity and Change in Patients with Erythropoietic Protoporphyria: The EPP Impact Questionnaire (EPIQ).Patient Relat Outcome Meas. 2024 Feb 14;15:17-30. doi: 10.2147/PROM.S438892. eCollection 2024. Patient Relat Outcome Meas. 2024. PMID: 38375415 Free PMC article.
-
Recognized and Emerging Features of Erythropoietic and X-Linked Protoporphyria.Diagnostics (Basel). 2022 Jan 8;12(1):151. doi: 10.3390/diagnostics12010151. Diagnostics (Basel). 2022. PMID: 35054318 Free PMC article. Review.
-
Increased phototoxic burn tolerance time and quality of life in patients with erythropoietic protoporphyria treated with afamelanotide - a three years observational study.Orphanet J Rare Dis. 2020 Aug 18;15(1):213. doi: 10.1186/s13023-020-01505-6. Orphanet J Rare Dis. 2020. PMID: 32811524 Free PMC article.
-
Afamelanotide in protoporphyria and other skin diseases: a review.Postepy Dermatol Alergol. 2024 Apr;41(2):149-154. doi: 10.5114/ada.2024.138818. Epub 2024 Apr 12. Postepy Dermatol Alergol. 2024. PMID: 38784937 Free PMC article. Review.
-
A case of erythrogenic protoporphyria with thyrotoxicosis and liver dysfunction in an adult female.Zhong Nan Da Xue Xue Bao Yi Xue Ban. 2023 Nov 28;48(11):1769-1774. doi: 10.11817/j.issn.1672-7347.2023.230242. Zhong Nan Da Xue Xue Bao Yi Xue Ban. 2023. PMID: 38432869 Free PMC article. Chinese, English.

