A Review of Von Hippel-Lindau Syndrome
- PMID: 28785532
- PMCID: PMC5541202
- DOI: 10.15586/jkcvhl.2017.88
A Review of Von Hippel-Lindau Syndrome
Abstract
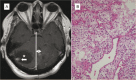
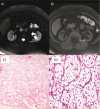
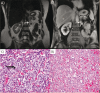
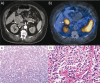
Von Hippel-Lindau syndrome (VHL) is a familial neoplastic condition seen in approximately 1 in 36,000 live births. It is caused by germline mutations of the tumor suppressor gene VHL, located on the short arm of chromosome 3. While the majority of the affected individuals have a positive family history, up to 20% of cases arise from de novo mutations. VHL syndrome is characterized by the presence of benign and malignant tumors affecting the central nervous system, kidneys, adrenals, pancreas, and reproductive organs. Common manifestations include hemangioblastomas of the brain, spinal cord, and retina; pheochromocytoma and paraganglioma; renal cell carcinoma; pancreatic cysts and neuroendocrine tumors; and endolymphatic sac tumors. Diagnosis of VHL is prompted by clinical suspicion and confirmed by molecular testing. Management of VHL patients is complex and multidisciplinary. Routine genetic testing and surveillance using various diagnostic techniques are used to help monitor disease progression and implement treatment options. Despite recent advances in clinical diagnosis and management, life expectancy for VHL patients remains low at 40-52 years. This article provides an overview of the major clinical, histological, and radiological findings, as well as treatment modalities.
Keywords: endolymphatic sac tumors; hemangioblastomas; pancreatic neuroendocrine tumors; pheochromocytoma; von Hippel-Lindau syndrome.
Figures
Similar articles
-
Von Hippel-Lindau syndrome. A pleomorphic condition.Cancer. 1999 Dec 1;86(11 Suppl):2478-82. Cancer. 1999. PMID: 10630173 Review.
-
Von Hippel-Lindau disease.Handb Clin Neurol. 2015;132:139-56. doi: 10.1016/B978-0-444-62702-5.00010-X. Handb Clin Neurol. 2015. PMID: 26564077 Free PMC article. Review.
-
[Von Hippel-Lindau syndrome - two sides of the same coin].Vnitr Lek. 2016 Winter;62(12):1004-1008. Vnitr Lek. 2016. PMID: 28139130 Review. Czech.
-
Von Hippel-Lindau disease: a single gene, several hereditary tumors.J Endocrinol Invest. 2018 Jan;41(1):21-31. doi: 10.1007/s40618-017-0683-1. Epub 2017 Jun 6. J Endocrinol Invest. 2018. PMID: 28589383 Review.
-
[Von Hippel-Lindau disease: recent genetic progress and patient management. Francophone Study Group of von Hippel-Lindau Disease (GEFVH)].Ann Endocrinol (Paris). 1998;59(6):452-8. Ann Endocrinol (Paris). 1998. PMID: 10189987 Review. French.
Cited by
-
Neurological applications of belzutifan in von Hippel-Lindau disease.Neuro Oncol. 2023 May 4;25(5):827-838. doi: 10.1093/neuonc/noac234. Neuro Oncol. 2023. PMID: 36215167 Free PMC article.
-
Single Stage Bilateral Adrenalectomy (Cortical-Sparing) and Pancreatectomy (Corpus-Sparing) in a Patient with Von Hippel-Lindau Disease.Sisli Etfal Hastan Tip Bul. 2024 Jun 28;58(2):233-236. doi: 10.14744/SEMB.2023.03743. eCollection 2024. Sisli Etfal Hastan Tip Bul. 2024. PMID: 39021689 Free PMC article.
-
Genetic Counseling and Long-Term Surveillance Using a Multidisciplinary Approach in von Hippel-Lindau Disease.Ann Lab Med. 2022 May 1;42(3):352-357. doi: 10.3343/alm.2022.42.3.352. Ann Lab Med. 2022. PMID: 34907105 Free PMC article.
-
Can Targeting Hypoxia-Mediated Acidification of the Bone Marrow Microenvironment Kill Myeloma Tumor Cells?Front Oncol. 2021 Jul 19;11:703878. doi: 10.3389/fonc.2021.703878. eCollection 2021. Front Oncol. 2021. PMID: 34350119 Free PMC article.
-
Induction of the Mdm2 gene and protein by kinase signaling pathways is repressed by the pVHL tumor suppressor.Proc Natl Acad Sci U S A. 2024 Jul 30;121(31):e2400935121. doi: 10.1073/pnas.2400935121. Epub 2024 Jul 24. Proc Natl Acad Sci U S A. 2024. PMID: 39047034 Free PMC article.
References
-
- Maher ER. Von Hippel-Lindau disease. Eur J Can. 1994. January;30(13):1987–90. http://dx.doi.org/10.1016/0959-8049(94)00391-H - DOI - PubMed
-
- Poulsen ML, Budtz-Jørgensen E, Bisgaard ML. Surveillance in von Hippel-Lindau disease (VHL). Clin Genet. 2010. January;77(1):49–59. http://dx.doi.org/10.1111/j.1399-0004.2009.01281.x - DOI - PubMed
-
- Wilding A, Ingham SL, Lalloo F, Clancy T, Huson SM, Moran A, et al. . Life expectancy in hereditary cancer predisposing diseases: An observational study. J Med Genet. 2012. April;49(4):264–9. http://dx.doi.org/10.1136/jmedgenet-2011-100562 - DOI - PubMed
-
- Iliopoulos O, Ohh M, Kaelin WG. pVHL19 is a biologically active product of the von Hippel-Lindau gene arising from internal translation initiation. Proc Natl Acad Sci U S A. 1998;95:11661–6. http://dx.doi.org/10.1073/pnas.95.20.11661 - DOI - PMC - PubMed
-
- Lonser RR, Glenn GM, Walther M, Chew EY, Libutti SK, Linehan WM, et al. . Von Hippel-Lindau disease. Lancet. 2003. June; 361(9374):2059–67. http://dx.doi.org/10.1016/S0140-6736(03)13643-4 - DOI - PubMed
Publication types
LinkOut - more resources
Full Text Sources
Other Literature Sources
