Irinotecan-temozolomide with temsirolimus or dinutuximab in children with refractory or relapsed neuroblastoma (COG ANBL1221): an open-label, randomised, phase 2 trial
- PMID: 28549783
- PMCID: PMC5527694
- DOI: 10.1016/S1470-2045(17)30355-8
Irinotecan-temozolomide with temsirolimus or dinutuximab in children with refractory or relapsed neuroblastoma (COG ANBL1221): an open-label, randomised, phase 2 trial
Abstract
Background: Outcomes for children with relapsed and refractory neuroblastoma are dismal. The combination of irinotecan and temozolomide has activity in these patients, and its acceptable toxicity profile makes it an excellent backbone for study of new agents. We aimed to test the addition of temsirolimus or dinutuximab to irinotecan-temozolomide in patients with relapsed or refractory neuroblastoma.
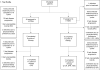
Methods: For this open-label, randomised, phase 2 selection design trial of the Children's Oncology Group (COG; ANBL1221), patients had to have histological verification of neuroblastoma or ganglioneuroblastoma at diagnosis or have tumour cells in bone marrow with increased urinary catecholamine concentrations at diagnosis. Patients of any age were eligible at first designation of relapse or progression, or first designation of refractory disease, provided organ function requirements were met. Patients previously treated for refractory or relapsed disease were ineligible. Computer-based randomisation with sequence generation defined by permuted block randomisation (block size two) was used to randomly assign patients (1:1) to irinotecan and temozolomide plus either temsirolimus or dinutuximab, stratified by disease category, previous exposure to anti-GD2 antibody therapy, and tumour MYCN amplification status. Patients in both groups received oral temozolomide (100 mg/m2 per dose) and intravenous irinotecan (50 mg/m2 per dose) on days 1-5 of 21-day cycles. Patients in the temsirolimus group also received intravenous temsirolimus (35 mg/m2 per dose) on days 1 and 8, whereas those in the dinutuximab group received intravenous dinutuximab (17·5 mg/m2 per day or 25 mg/m2 per day) on days 2-5 plus granulocyte macrophage colony-stimulating factor (250 μg/m2 per dose) subcutaneously on days 6-12. Patients were given up to a maximum of 17 cycles of treatment. The primary endpoint was the proportion of patients achieving an objective (complete or partial) response by central review after six cycles of treatment, analysed by intention to treat. Patients, families, and those administering treatment were aware of group assignment. This study is registered with ClinicalTrials.gov, number NCT01767194, and follow-up of the initial cohort is ongoing.
Findings: Between Feb 22, 2013, and March 23, 2015, 36 patients from 27 COG member institutions were enrolled on this groupwide study. One patient was ineligible (alanine aminotransferase concentration was above the required range). Of the remaining 35 patients, 18 were randomly assigned to irinotecan-temozolomide-temsirolimus and 17 to irinotecan-temozolomide-dinutuximab. Median follow-up was 1·26 years (IQR 0·68-1·61) among all eligible participants. Of the 18 patients assigned to irinotecan-temozolomide-temsirolimus, one patient (6%; 95% CI 0·0-16·1) achieved a partial response. Of the 17 patients assigned to irinotecan-temozolomide-dinutuximab, nine (53%; 95% CI 29·2-76·7) had objective responses, including four partial responses and five complete responses. The most common grade 3 or worse adverse events in the temsirolimus group were neutropenia (eight [44%] of 18 patients), anaemia (six [33%]), thrombocytopenia (five [28%]), increased alanine aminotransferase (five [28%]), and hypokalaemia (four [22%]). One of the 17 patients assigned to the dinutuximab group refused treatment after randomisation; the most common grade 3 or worse adverse events in the remaining 16 patients evaluable for safety were pain (seven [44%] of 16), hypokalaemia (six [38%]), neutropenia (four [25%]), thrombocytopenia (four [25%]), anaemia (four [25%]), fever and infection (four [25%]), and hypoxia (four [25%]); one patient had grade 4 hypoxia related to therapy that met protocol-defined criteria for unacceptable toxicity. No deaths attributed to protocol therapy occurred.
Interpretation: Irinotecan-temozolomide-dinutuximab met protocol-defined criteria for selection as the combination meriting further study whereas irinotecan-temozolomide-temsirolimus did not. Irinotecan-temozolomide-dinutuximab shows notable anti-tumour activity in patients with relapsed or refractory neuroblastoma. Further evaluation of biomarkers in a larger cohort of patients might identify those most likely to respond to this chemoimmunotherapeutic regimen.
Funding: National Cancer Institute.
Copyright © 2017 Elsevier Ltd. All rights reserved.
Figures


Comment in
-
Chemoimmunotherapy for high-risk neuroblastoma.Lancet Oncol. 2017 Jul;18(7):845-846. doi: 10.1016/S1470-2045(17)30337-6. Epub 2017 May 23. Lancet Oncol. 2017. PMID: 28549784 No abstract available.
Similar articles
-
Irinotecan and temozolomide in combination with dasatinib and rapamycin versus irinotecan and temozolomide for patients with relapsed or refractory neuroblastoma (RIST-rNB-2011): a multicentre, open-label, randomised, controlled, phase 2 trial.Lancet Oncol. 2024 Jul;25(7):922-932. doi: 10.1016/S1470-2045(24)00202-X. Lancet Oncol. 2024. PMID: 38936379 Clinical Trial.
-
Irinotecan, Temozolomide, and Dinutuximab With GM-CSF in Children With Refractory or Relapsed Neuroblastoma: A Report From the Children's Oncology Group.J Clin Oncol. 2020 Jul 1;38(19):2160-2169. doi: 10.1200/JCO.20.00203. Epub 2020 Apr 28. J Clin Oncol. 2020. PMID: 32343642 Free PMC article. Clinical Trial.
-
Interleukin 2 with anti-GD2 antibody ch14.18/CHO (dinutuximab beta) in patients with high-risk neuroblastoma (HR-NBL1/SIOPEN): a multicentre, randomised, phase 3 trial.Lancet Oncol. 2018 Dec;19(12):1617-1629. doi: 10.1016/S1470-2045(18)30578-3. Epub 2018 Nov 12. Lancet Oncol. 2018. PMID: 30442501 Clinical Trial.
-
Historical time to disease progression and progression-free survival in patients with recurrent/refractory neuroblastoma treated in the modern era on Children's Oncology Group early-phase trials.Cancer. 2017 Dec 15;123(24):4914-4923. doi: 10.1002/cncr.30934. Epub 2017 Sep 8. Cancer. 2017. PMID: 28885700 Free PMC article. Review.
-
Dinutuximab for maintenance therapy in pediatric neuroblastoma.Am J Health Syst Pharm. 2017 Apr 15;74(8):563-567. doi: 10.2146/ajhp160228. Am J Health Syst Pharm. 2017. PMID: 28389455 Review.
Cited by
-
The Emerging Role of Ras Pathway Signaling in Pediatric Cancer.Cancer Res. 2020 Dec 1;80(23):5155-5163. doi: 10.1158/0008-5472.CAN-20-0916. Epub 2020 Sep 9. Cancer Res. 2020. PMID: 32907837 Free PMC article. Review.
-
Comprehensive understanding of the adverse effects associated with temozolomide: a disproportionate analysis based on the FAERS database.Front Pharmacol. 2024 Aug 23;15:1437436. doi: 10.3389/fphar.2024.1437436. eCollection 2024. Front Pharmacol. 2024. PMID: 39246656 Free PMC article.
-
Phase 2 study of anti-disialoganglioside antibody, dinutuximab, in combination with GM-CSF in patients with recurrent osteosarcoma: A report from the Children's Oncology Group.Eur J Cancer. 2022 Sep;172:264-275. doi: 10.1016/j.ejca.2022.05.035. Epub 2022 Jul 6. Eur J Cancer. 2022. PMID: 35809374 Free PMC article. Clinical Trial.
-
Mechanisms, Characteristics, and Treatment of Neuropathic Pain and Peripheral Neuropathy Associated with Dinutuximab in Neuroblastoma Patients.Int J Mol Sci. 2021 Nov 23;22(23):12648. doi: 10.3390/ijms222312648. Int J Mol Sci. 2021. PMID: 34884452 Free PMC article. Review.
-
Neuroblastoma: clinical and biological approach to risk stratification and treatment.Cell Tissue Res. 2018 May;372(2):195-209. doi: 10.1007/s00441-018-2821-2. Epub 2018 Mar 23. Cell Tissue Res. 2018. PMID: 29572647 Free PMC article. Review.
References
-
- Kushner BH, Kramer K, Modak S, Cheung NK. Irinotecan plus temozolomide for relapsed or refractory neuroblastoma. J Clin Oncol. 2006;24(33):5271–6. - PubMed
-
- Johnsen JI, Segerstrom L, Orrego A, Elfman L, Henriksson M, Kagedal B, et al. Inhibitors of mammalian target of rapamycin downregulate MYCN protein expression and inhibit neuroblastoma growth in vitro and in vivo. Oncogene. 2008;27(20):2910–22. - PubMed
Publication types
MeSH terms
Substances
Associated data
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Miscellaneous

