Advances in the management of erythropoietic protoporphyria - role of afamelanotide
- PMID: 28003770
- PMCID: PMC5161401
- DOI: 10.2147/TACG.S122030
Advances in the management of erythropoietic protoporphyria - role of afamelanotide
Abstract
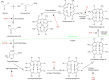
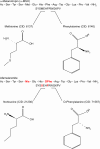
Erythropoietic protoporphyria (EPP) and the phenotypically similar disease X-linked protoporphyria (XLPP) are inherited cutaneous porphyrias characterized clinically by acute non-blistering photosensitivity, intolerance to sunlight, and significantly reduced quality of life. They are due to marked overproduction of protoporphyrin (PP) chiefly by erythroblasts and reticulocytes. In EPP, the underlying genetic defect is in the ferrochelatase gene, which encodes the final enzyme in the heme synthetic pathway. In XLPP, the genetic defect is a gain-of-function mutation, usually a four-base deletion, in the gene that encodes the enzyme 5-aminolevulinic acid synthase-2, the first and rate-controlling enzyme of heme synthesis in developing red blood cells. The excess PP causes acute and painful photosensitivity, being activated by light in the long ultraviolet to blue spectrum (380-420 nm, the Soret band). Although several treatments have been proposed, presently no very effective treatment exists for EPP or XLPP. Afamelanotide (Scenesse®) is a first-in-class synthetic analog of α-melanocyte stimulating hormone. Afamelanotide mimics the naturally occurring hormone to increase skin pigmentation by increasing melanin production in melanocytes, resulting in increased sunlight tolerance in those with EPP/XLPP. Afamelanotide is currently approved for use in the European Union and Switzerland, and it is under review in the United States by the Food and Drug Administration for use in patients with EPP/XLPP. This paper provides a review of the clinical characteristics and current therapies for EPP/XLPP. We discuss the pharmacology, clinical efficacy, safety, and tolerability of afamelanotide and summarize the results of several key Phase II and III clinical trials. These data indicate that afamelanotide is a promising therapy for those with these debilitating diseases.
Keywords: afamelanotide; eumelanin; heme; melanocyte stimulating hormone; photosensitivity; porphyria.
Conflict of interest statement
Within the past 3 years, Dr Bonkovsky has received research funding from Alnylam Pharma. He has served as a consultant to Alnylam Pharma, Clinuvel, Recordati Rare Chemicals, and Mitsubishi-Tanabe. The authors report no other conflicts of interest in this work.
Figures



Similar articles
-
Beyond pigmentation: signs of liver protection during afamelanotide treatment in Swiss patients with erythropoietic protoporphyria, an observational study.Ther Adv Rare Dis. 2021 Dec 21;2:26330040211065453. doi: 10.1177/26330040211065453. eCollection 2021 Jan-Dec. Ther Adv Rare Dis. 2021. PMID: 37181106 Free PMC article.
-
Afamelanotide for prevention of phototoxicity in erythropoietic protoporphyria.Expert Rev Clin Pharmacol. 2021 Feb;14(2):151-160. doi: 10.1080/17512433.2021.1879638. Expert Rev Clin Pharmacol. 2021. PMID: 33507118 Review.
-
Afamelanotide in protoporphyria and other skin diseases: a review.Postepy Dermatol Alergol. 2024 Apr;41(2):149-154. doi: 10.5114/ada.2024.138818. Epub 2024 Apr 12. Postepy Dermatol Alergol. 2024. PMID: 38784937 Free PMC article. Review.
-
Afamelanotide: A Review in Erythropoietic Protoporphyria.Am J Clin Dermatol. 2016 Apr;17(2):179-85. doi: 10.1007/s40257-016-0184-6. Am J Clin Dermatol. 2016. PMID: 26979527 Review.
-
Erythropoietic Protoporphyria and X-Linked Protoporphyria: pathophysiology, genetics, clinical manifestations, and management.Mol Genet Metab. 2019 Nov;128(3):298-303. doi: 10.1016/j.ymgme.2019.01.020. Epub 2019 Jan 24. Mol Genet Metab. 2019. PMID: 30704898 Free PMC article. Review.
Cited by
-
Cockayne syndrome group A and ferrochelatase finely tune ribosomal gene transcription and its response to UV irradiation.Nucleic Acids Res. 2021 Nov 8;49(19):10911-10930. doi: 10.1093/nar/gkab819. Nucleic Acids Res. 2021. PMID: 34581821 Free PMC article.
-
5-Aminolevulinate synthase catalysis: The catcher in heme biosynthesis.Mol Genet Metab. 2019 Nov;128(3):178-189. doi: 10.1016/j.ymgme.2019.06.003. Epub 2019 Jun 13. Mol Genet Metab. 2019. PMID: 31345668 Free PMC article. Review.
-
Journey through the spectacular landscape of melanocortin 1 receptor.Pigment Cell Melanoma Res. 2024 Sep;37(5):667-680. doi: 10.1111/pcmr.13180. Epub 2024 Jun 10. Pigment Cell Melanoma Res. 2024. PMID: 38857302 Review.
-
Iron Hack - A symposium/hackathon focused on porphyrias, Friedreich's ataxia, and other rare iron-related diseases.F1000Res. 2019 Jul 19;8:1135. doi: 10.12688/f1000research.19140.1. eCollection 2019. F1000Res. 2019. PMID: 31824661 Free PMC article.
-
Regulation of protein function and degradation by heme, heme responsive motifs, and CO.Crit Rev Biochem Mol Biol. 2022 Feb;57(1):16-47. doi: 10.1080/10409238.2021.1961674. Epub 2021 Sep 13. Crit Rev Biochem Mol Biol. 2022. PMID: 34517731 Free PMC article. Review.
References
-
- Todd DJ. Erythropoietic protoporphyria. Br J Dermatol. 1994;131(6):751–766. - PubMed
-
- Bonkovsky HL, Guo JT, Hou W, Li T, Narang T, Thapar M. Porphyrin and heme metabolism and the porphyrias. Compr Physiol. 2013;3(1):365–401. - PubMed
-
- Balwani M, Bloomer J, Desnick R, Porphyrias Consortium of the NIH-Sponsored Rare Diseases Clinical Research Network . Erythropoietic Protoporphyria, Autosomal Recessive. In: Pagon RA, Adam MP, Ardinger HH, et al., editors. GeneReviews® [Internet] Seattle (WA): University of Washington, Seattle; 2012. Sep 27, 1993–2016. Updated 2014 Oct 16. Available from: https://www.ncbi.nlm.nih.gov/books/NBK100826/ - PubMed
-
- Puy H, Gouya L, Deybach JC. Porphyrias. Lancet. 2010;375(9718):924–937. - PubMed
Publication types
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Miscellaneous

