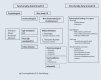
Modern diagnosis of celiac disease and relevant differential diagnoses in the case of cereal intolerance
- PMID: 26120517
- PMCID: PMC4479435
- DOI: 10.1007/s40629-014-0006-4
Modern diagnosis of celiac disease and relevant differential diagnoses in the case of cereal intolerance
Abstract
At an incidence of 1:500, celiac disease (formerly sprue) is an important differential diagnosis in patients with malabsorption, abdominal discomfort, diarrhea and food intolerances. Celiac disease can induce a broad spectrum of both gastrointestinal and extraintestinal symptoms, e.g. dermatitis herpetiformis (Duhring's disease). A variety of oligo- and asymptomatic courses (e.g. anemia, osteoporosis, depression) through to refractory collagenic celiac disease are seen. In HLA-DQ2 and -8 predisposed individuals, celiac disease is provoked by contact with wheat gliadin fractions through a predominantly Th1 immune response and an accompanying Th2 response, which can eventually lead to villous atrophy. Using appropriate serological tests (IgA antibodies against tissue-transglutaminase, endomysium and deamidated gliadin peptides) under sufficient gluten ingestion, the diagnosis can be made more reliably today than previously. The same IgG-based serological tests should be used in the case of IgA deficiency. Diagnosis can either be made in children and adolescents with anti-transglutaminase titers exceeding ten times the standard for two of the above-mentioned serological markers and HLA conformity or it is made by endoscopy and histological Marsh classification in adults and in cases of inconclusive serology. If clinically tolerated, gluten challenges are indicated in patients that already have reduced gluten intake, in borderline serological results, discordance between serological and histological results or in suspected food allergy. The diagnosis of celiac disease needs to be definitive and robust before establishing a gluten-free diet, since lifelong abstention from gluten (gliadin < 20 mg/kg foodstuffs), cereal products (wheat, rye, barley and spelt) as well as from preparations and beverages containing gluten, is necessary. With effective elimination of gluten, the prognosis regarding complete resolution of small bowel inflammation is good. Refractory courses are seen only in rare cases, accompanied by enteropathy-associated T-cell lymphoma.
Keywords: Celiac disease; cereal intolerance; enteropathy; malabsorption; sprue.
Figures
Similar articles
-
Celiac sprue.Semin Gastrointest Dis. 2002 Oct;13(4):232-44. Semin Gastrointest Dis. 2002. PMID: 12462708 Review.
-
Monitoring nonresponsive patients who have celiac disease.Gastrointest Endosc Clin N Am. 2006 Apr;16(2):317-27. doi: 10.1016/j.giec.2006.03.005. Gastrointest Endosc Clin N Am. 2006. PMID: 16644460 Review.
-
Celiac disease: risk assessment, diagnosis, and monitoring.Mol Diagn Ther. 2008;12(5):289-98. doi: 10.1007/BF03256294. Mol Diagn Ther. 2008. PMID: 18803427 Review.
-
Celiac disease in children.Clin Res Hepatol Gastroenterol. 2015 Oct;39(5):544-51. doi: 10.1016/j.clinre.2015.05.024. Epub 2015 Jul 15. Clin Res Hepatol Gastroenterol. 2015. PMID: 26186878 Review.
-
Accuracy in Diagnosis of Celiac Disease Without Biopsies in Clinical Practice.Gastroenterology. 2017 Oct;153(4):924-935. doi: 10.1053/j.gastro.2017.06.002. Epub 2017 Jun 15. Gastroenterology. 2017. PMID: 28624578
Cited by
-
Concurrent cerebral arterial and venous sinus thrombosis revealing celiac disease- a case report and literature review.BMC Gastroenterol. 2020 Oct 6;20(1):327. doi: 10.1186/s12876-020-01483-w. BMC Gastroenterol. 2020. PMID: 33023506 Free PMC article. Review.
-
Pathogenesis of Celiac Disease and Other Gluten Related Disorders in Wheat and Strategies for Mitigating Them.Front Nutr. 2020 Feb 7;7:6. doi: 10.3389/fnut.2020.00006. eCollection 2020. Front Nutr. 2020. PMID: 32118025 Free PMC article. Review.
References
-
- Biesiekierski JR, Newnham ED, Irving PM, Barrett JS, Haines M, Doecke JD, Shepherd SJ, Muir JG, Gibson PR. Gluten causes gastrointestinal symptoms in subjects without celiac disease: a double-blind randomized placebo-controlled trial. Am J Gastroenterol. 2011;106:508–14. doi: 10.1038/ajg.2010.487. - DOI - PubMed
Publication types
LinkOut - more resources
Full Text Sources
Other Literature Sources
Research Materials
Miscellaneous