Impact of preoperative MRSA screening and decolonization on hospital-acquired MRSA burden
- PMID: 23423618
- PMCID: PMC3676612
- DOI: 10.1007/s11999-013-2848-3
Impact of preoperative MRSA screening and decolonization on hospital-acquired MRSA burden
Erratum in
- Clin Orthop Relat Res. 2013 Jun;471(6):2044
Abstract
Background: Hospital-acquired infections caused by methicillin-resistant Staphylococcus aureus (MRSA) are a source of morbidity and mortality. S. aureus is the most common pathogen in prosthetic joint infections and the incidence of MRSA is increasing.
Questions/purposes: The purposes of this study were (1) to determine the MRSA prevalence density rate at a specialty orthopaedic hospital before and after the implementation of a screening and decolonization protocol,(2) to compare our prevalence density to that of an affiliated university hospital, to control for changes in MRSA prevalence density that might have been independent of the decolonization protocol, and (3) to measure the admission prevalence density rate of MRSA in an elective orthopaedic surgery population and the compliance rate of 26 patients with the protocol [corrected].
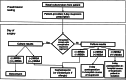
Methods: In October 2008, we implemented a MRSA screening and decolonization protocol for patients undergoing elective orthopaedic surgery. Nasal swabs were used for screening and mupirocin nasal ointment and chlorhexidine skin antisepsis where prescribed for decolonization to all patients. At the surgical visit, compliance was measured and the patients who were MRSA positive received vancomycin for antibiotic prophylaxis. Institution wide surveillance for multidrug-resistant organisms, including MRSA provided a comparison of the change in MRSA burden at the orthopaedic hospital versus the university hospital.
Results: Before implementation of the preoperative staphylococcal decolonization protocol there were 79 MRSA-positive cultures in 64,327 patient-days for a prevalence density rate of 1.23 per 1000 patient-days. After protocol implementation, 53 MRSA-positive cultures were identified in 63,860 patient-days for a rate of 0.83 per 1000 patient-days. Before the protocol, the MRSA prevalence density at the specialty hospital was similar to that of the university hospital; after implementation of the protocol, the prevalence density at the specialty hospital was 33% lower than that of the university hospital. The MRSA admission prevalence was 3.02%. The compliance rate was greater than 95%.
Conclusions: Implementation of a staphylococcal decolonization protocol at a single specialty orthopaedic hospital decreased the prevalence density of MRSA.
Figures
Comment in
-
CORR Insights®: Impact of preoperative MRSA screening and decolonization on hospital-acquired MRSA burden.Clin Orthop Relat Res. 2013 Jul;471(7):2372-3. doi: 10.1007/s11999-013-2909-7. Epub 2013 May 21. Clin Orthop Relat Res. 2013. PMID: 23690147 Free PMC article. No abstract available.
Similar articles
-
Staphylococcus aureus screening and decolonization in orthopaedic surgery and reduction of surgical site infections.Clin Orthop Relat Res. 2013 Jul;471(7):2383-99. doi: 10.1007/s11999-013-2875-0. Epub 2013 Mar 6. Clin Orthop Relat Res. 2013. PMID: 23463284 Free PMC article. Review.
-
The Impact of a Universal Decolonization Protocol on Hospital-Acquired Methicillin-Resistant Staphylococcus aureus in a Burn Population.J Burn Care Res. 2016 Nov/Dec;37(6):e525-e530. doi: 10.1097/BCR.0000000000000301. J Burn Care Res. 2016. PMID: 27828836
-
CORR Insights®: Impact of preoperative MRSA screening and decolonization on hospital-acquired MRSA burden.Clin Orthop Relat Res. 2013 Jul;471(7):2372-3. doi: 10.1007/s11999-013-2909-7. Epub 2013 May 21. Clin Orthop Relat Res. 2013. PMID: 23690147 Free PMC article. No abstract available.
-
Methicillin-Resistant and Methicillin-Sensitive Staphylococcus aureus Screening and Decolonization to Reduce Surgical Site Infection in Elective Total Joint Arthroplasty.J Arthroplasty. 2016 Sep;31(9 Suppl):144-7. doi: 10.1016/j.arth.2016.05.019. Epub 2016 May 18. J Arthroplasty. 2016. PMID: 27387479 Clinical Trial.
-
Agents for the decolonization of methicillin-resistant Staphylococcus aureus.Pharmacotherapy. 2009 Mar;29(3):263-80. doi: 10.1592/phco.29.3.263. Pharmacotherapy. 2009. PMID: 19249946 Review.
Cited by
-
Effectiveness of Extended Infection Control Measures on Methicillin-Resistant Staphylococcus aureus Infection Among Orthopaedic Patients.Indian J Orthop. 2022 Aug 20;56(10):1804-1812. doi: 10.1007/s43465-022-00713-5. eCollection 2022 Oct. Indian J Orthop. 2022. PMID: 36187590 Free PMC article.
-
Comparative Effectiveness Study of Home-Based Interventions to Prevent CA-MRSA Infection Recurrence.Antibiotics (Basel). 2021 Sep 13;10(9):1105. doi: 10.3390/antibiotics10091105. Antibiotics (Basel). 2021. PMID: 34572687 Free PMC article.
-
Do lower respiratory tract samples contribute to the assessment of carriage of Staphylococcus aureus in patients undergoing mechanical ventilation after major heart surgery?PLoS One. 2018 Dec 26;13(12):e0207854. doi: 10.1371/journal.pone.0207854. eCollection 2018. PLoS One. 2018. PMID: 30586363 Free PMC article.
-
An update on the best approaches to prevent complications in penile prosthesis recipients.Ther Adv Urol. 2019 Jan 8;11:1756287218818076. doi: 10.1177/1756287218818076. eCollection 2019 Jan-Dec. Ther Adv Urol. 2019. PMID: 30671142 Free PMC article. Review.
-
Health care-associated infections in children after cardiac surgery.Pediatr Cardiol. 2014 Dec;35(8):1448-55. doi: 10.1007/s00246-014-0953-z. Epub 2014 Jul 5. Pediatr Cardiol. 2014. PMID: 24996642
References
-
- Bode LG, Kluytmans JA, Wertheim HF, Bogaers D, Vandenbroucke-Grauls CM, Roosendaal R, Troelstra A, Box AT, Voss A, van der Tweel I, van Belkum A, Verbrugh HA, Vos MC. Preventing surgical-site infections in nasal carriers of Staphylococcus aureus. N Engl J Med. 2010;362:9–17. doi: 10.1056/NEJMoa0808939. - DOI - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

