Ductal adenocarcinoma of the pancreatic head: a focus on current diagnostic and surgical concepts
- PMID: 22791941
- PMCID: PMC3386319
- DOI: 10.3748/wjg.v18.i24.3058
Ductal adenocarcinoma of the pancreatic head: a focus on current diagnostic and surgical concepts
Abstract
Complete surgical resection still remains the only possibility of curing pancreatic cancer, however, only 10% of patients undergo curative surgery. Pancreatic resection currently remains the only method of curing patients, and has a 5-year overall survival rate between 7%-34% compared to a median survival of 3-11 mo for unresected cancer. Pancreatic surgery is a technically demanding procedure requiring highly standardized surgical techniques. Nevertheless, even in experienced hands, perioperative morbidity rates (delayed gastric emptying, pancreatic fistula etc.) are as high as 50%. Different strategies to reduce postoperative morbidity, such as different techniques of gastroenteric reconstruction (pancreatico-jejunostomy vs pancreatico-gastrostomy), intraoperative placement of a pancreatic main duct stent or temporary sealing of the main pancreatic duct with fibrin glue have not led to a significant improvement in clinical outcome. The perioperative application of somatostatin or its analogues may decrease the incidence of pancreatic fistulas in cases with soft pancreatic tissue and a small main pancreatic duct (< 3 mm). The positive effects of external pancreatic main duct drainage and antecolic gastrointestinal reconstruction have been observed to decrease the rate of pancreatic fistulas and delayed gastric emptying, respectively. Currently, the concept of extended radical lymphadenectomy has been found to be associated with higher perioperative morbidity, but without any positive impact on overall survival. However, there is growing evidence that portal vein resections can be performed with acceptable low perioperative morbidity and mortality but does not achieve a cure.
Keywords: Pancreatic adenocarcinoma; Pancreatic fistula; Pancreatic surgery; Venous resection.
Figures
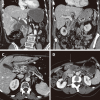
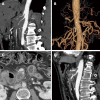
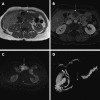
Similar articles
-
[New aspects of surgery for pancreatic cancer. Principles, results and evidence].Pathologe. 2012 Nov;33 Suppl 2:258-65. doi: 10.1007/s00292-012-1639-z. Pathologe. 2012. PMID: 23108784 Review. German.
-
[Surgery of malignant pancreatic tumors].Radiologe. 2009 Feb;49(2):137-43. doi: 10.1007/s00117-008-1752-4. Radiologe. 2009. PMID: 19153706 Review. German.
-
International Study Group of Pancreatic Surgery type 3 and 4 venous resections in patients with pancreatic adenocarcinoma:the Paoli-Calmettes Institute experience.Eur J Surg Oncol. 2019 Oct;45(10):1912-1918. doi: 10.1016/j.ejso.2019.06.003. Epub 2019 Jun 3. Eur J Surg Oncol. 2019. PMID: 31186204
-
Long-term outcomes following en bloc resection for pancreatic ductal adenocarcinoma of the head with portomesenteric venous invasion.Asian J Surg. 2021 Jan;44(1):313-320. doi: 10.1016/j.asjsur.2020.07.021. Epub 2020 Sep 21. Asian J Surg. 2021. PMID: 32972828
-
Pancreatic head resection with segmental duodenectomy: safety and long-term results.Ann Surg. 2007 Dec;246(6):923-8; discussion 929-31. doi: 10.1097/SLA.0b013e31815c2a14. Ann Surg. 2007. PMID: 18043093
Cited by
-
Connexins and pannexins in the skeleton: gap junctions, hemichannels and more.Cell Mol Life Sci. 2015 Aug;72(15):2853-67. doi: 10.1007/s00018-015-1963-6. Epub 2015 Jun 20. Cell Mol Life Sci. 2015. PMID: 26091748 Free PMC article. Review.
-
Novel diagnostics for aggravating pancreatic fistulas at the acute phase after pancreatectomy.World J Gastroenterol. 2014 Jul 14;20(26):8535-44. doi: 10.3748/wjg.v20.i26.8535. World J Gastroenterol. 2014. PMID: 25024608 Free PMC article.
-
Pancreatic fistulae after a pancreatico-duodenectomy: are pancreatico-gastrostomies safer than pancreatico-jejunostomies? An expertise-based trial and propensity-score adjusted analysis.HPB (Oxford). 2014 Dec;16(12):1062-7. doi: 10.1111/hpb.12294. Epub 2014 Jun 19. HPB (Oxford). 2014. PMID: 24946170 Free PMC article.
-
Impact of body mass index on complications following pancreatectomy: Ten-year experience at National Cancer Center in China.World J Gastroenterol. 2015 Jun 21;21(23):7218-24. doi: 10.3748/wjg.v21.i23.7218. World J Gastroenterol. 2015. PMID: 26109808 Free PMC article.
-
Biliary Tract Carcinogenesis Model Based on Bile Metaproteomics.Front Oncol. 2020 Jul 24;10:1032. doi: 10.3389/fonc.2020.01032. eCollection 2020. Front Oncol. 2020. PMID: 32793466 Free PMC article.
References
-
- Jemal A, Thomas A, Murray T, Thun M. Cancer statistics, 2002. CA Cancer J Clin. 2002;52:23–47. - PubMed
-
- Ouaissi M, Hubert C, Verhelst R, Astarci P, Sempoux C, Jouret-Mourin A, Loundou A, Gigot JF. Vascular reconstruction during pancreatoduodenectomy for ductal adenocarcinoma of the pancreas improves resectability but does not achieve cure. World J Surg. 2010;34:2648–2661. - PubMed
-
- Baumel H, Huguier M, Manderscheid JC, Fabre JM, Houry S, Fagot H. Results of resection for cancer of the exocrine pancreas: a study from the French Association of Surgery. Br J Surg. 1994;81:102–107. - PubMed
-
- Delpero JR, Paye F, Bachellier P. Cancer du pancréas, Monographies de l'Association française de chirurgie. Paris: Wolters Kluwer France; 2010.
-
- Oettle H, Post S, Neuhaus P, Gellert K, Langrehr J, Ridwelski K, Schramm H, Fahlke J, Zuelke C, Burkart C, et al. Adjuvant chemotherapy with gemcitabine vs observation in patients undergoing curative-intent resection of pancreatic cancer: a randomized controlled trial. JAMA. 2007;297:267–277. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

