Role of 18F-fluorodeoxyglucose positron emission tomography imaging in surgery for pancreatic cancer
- PMID: 18176963
- PMCID: PMC2673393
- DOI: 10.3748/wjg.14.64
Role of 18F-fluorodeoxyglucose positron emission tomography imaging in surgery for pancreatic cancer
Abstract
Aim: To evaluate the role of positron emission tomography using 18F-fluorodeoxyglucose (FDG-PET) in the surgical management of patients with pancreatic cancer, including the diagnosis, staging, and selection of patients for the subsequent surgical treatment.
Methods: This study involved 53 patients with proven primary pancreatic cancer. The sensitivity of diagnosing the primary cancer was examined for FDG-PET, CT, cytological examination of the bile or pancreatic juice, and the serum levels of carcinoembrionic antigens (CEA) and carbohydrate antigen 19-9 (CA19-9). Next, the accuracy of staging was compared between FDG-PET and CT. Finally, FDG-PET was analyzed semiquantitatively using the standard uptake value (SUV). The impact of the SUV on patient management was evaluated by examining the correlations between the SUV and the histological findings of cancer.
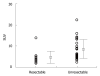
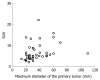
Results: The sensitivity of FDG-PET, CT, cytological examination of the bile or pancreatic juice, and the serum levels of CEA and CA19-9 were 92.5%, 88.7%, 46.4%, 37.7% and 69.8%, respectively. In staging, FDG-PET was superior to CT only in diagnosing distant disease (bone metastasis). For local staging, the sensitivity of CT was better than that of FDG-PET. The SUV did not correlate with the pTNM stage, grades, invasions to the vessels and nerve, or with the size of the tumor. However, there was a statistically significant difference (4.6 +/- 2.9 vs 7.8 +/- 4.5, P = 0.024) in the SUV between patients with respectable and unresectable disease.
Conclusion: FDG-PET is thus considered to be useful in the diagnosis of pancreatic cancer. However, regarding the staging of the disease, FDG-PET is not considered to be a sufficiently accurate diagnostic modality. Although the SUV does not correlate with the patho-histological prognostic factors, it may be useful in selecting patients who should undergo subsequent surgical treatment.
Figures
Similar articles
-
Optimal interpretation of FDG PET in the diagnosis, staging and management of pancreatic carcinoma.J Nucl Med. 1999 Nov;40(11):1784-91. J Nucl Med. 1999. PMID: 10565771
-
[The application of 18F-fluorodeoxyglucose positron emission tomography in the diagnosis and staging of lung cancer].Zhonghua Jie He He Hu Xi Za Zhi. 2005 Feb;28(2):108-11. Zhonghua Jie He He Hu Xi Za Zhi. 2005. PMID: 15854393 Chinese.
-
Clinical impact of fluorine-18-fluorodeoxyglucose positron emission tomography/computed tomography in patients with resectable pancreatic cancer: diagnosing lymph node metastasis and predicting survival.Nucl Med Commun. 2018 Jul;39(7):691-698. doi: 10.1097/MNM.0000000000000855. Nucl Med Commun. 2018. PMID: 29893751
-
Usefulness of F-18-fluorodeoxyglucose positron emission tomography to confirm suspected pancreatic cancer: a meta-analysis.Eur J Surg Oncol. 2014 Jul;40(7):794-804. doi: 10.1016/j.ejso.2014.03.016. Epub 2014 Apr 3. Eur J Surg Oncol. 2014. PMID: 24755095 Review.
-
Hyperaccumulation of (18)F-FDG in order to differentiate solid pseudopapillary tumors from adenocarcinomas and from neuroendocrine pancreatic tumors and review of the literature.Hell J Nucl Med. 2013 May-Aug;16(2):97-102. doi: 10.1967/s002449910084. Epub 2013 May 20. Hell J Nucl Med. 2013. PMID: 23687644 Review.
Cited by
-
Utility of PET/CT in diagnosis, staging, assessment of resectability and metabolic response of pancreatic cancer.World J Gastroenterol. 2014 Nov 14;20(42):15580-9. doi: 10.3748/wjg.v20.i42.15580. World J Gastroenterol. 2014. PMID: 25400441 Free PMC article. Review.
-
The clinical usefulness of 18F-fluorodeoxyglucose positron emission tomography-computed tomography (PET-CT) in follow-up of curatively resected pancreatic cancer patients.HPB (Oxford). 2016 Jan;18(1):57-64. doi: 10.1016/j.hpb.2015.06.001. Epub 2015 Dec 21. HPB (Oxford). 2016. PMID: 26776852 Free PMC article.
-
Imaging modalities for characterising focal pancreatic lesions.Cochrane Database Syst Rev. 2017 Apr 17;4(4):CD010213. doi: 10.1002/14651858.CD010213.pub2. Cochrane Database Syst Rev. 2017. PMID: 28415140 Free PMC article. Review.
-
Cross-modality PET/CT and contrast-enhanced CT imaging for pancreatic cancer.World J Gastroenterol. 2015 Mar 14;21(10):2988-96. doi: 10.3748/wjg.v21.i10.2988. World J Gastroenterol. 2015. PMID: 25780297 Free PMC article.
-
Clinical value of serum CA19-9 levels in evaluating resectability of pancreatic carcinoma.World J Gastroenterol. 2008 Jun 21;14(23):3750-3. doi: 10.3748/wjg.14.3750. World J Gastroenterol. 2008. PMID: 18595144 Free PMC article.
References
-
- Li D, Xie K, Wolff R, Abbruzzese JL. Pancreatic cancer. Lancet. 2004;363:1049–1057. - PubMed
-
- Pakzad F, Groves AM, Ell PJ. The role of positron emission tomography in the management of pancreatic cancer. Semin Nucl Med. 2006;36:248–256. - PubMed
-
- Oettle H, Post S, Neuhaus P, Gellert K, Langrehr J, Ridwelski K, Schramm H, Fahlke J, Zuelke C, Burkart C, et al. Adjuvant chemotherapy with gemcitabine vs observation in patients undergoing curative-intent resection of pancreatic cancer: a randomized controlled trial. JAMA. 2007;297:267–277. - PubMed
-
- Nakata B, Nishimura S, Ishikawa T, Ohira M, Nishino H, Kawabe J, Ochi H, Hirakawa K. Prognostic predictive value of 18F-fluorodeoxyglucose positron emission tomography for patients with pancreatic cancer. Int J Oncol. 2001;19:53–58. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical