Defective high-affinity thiamine transporter leads to cell death in thiamine-responsive megaloblastic anemia syndrome fibroblasts
- PMID: 10074490
- PMCID: PMC408117
- DOI: 10.1172/JCI3895
Defective high-affinity thiamine transporter leads to cell death in thiamine-responsive megaloblastic anemia syndrome fibroblasts
Abstract
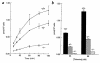
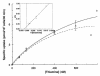
We have investigated the cellular pathology of the syndrome called thiamine-responsive megaloblastic anemia (TRMA) with diabetes and deafness. Cultured diploid fibroblasts were grown in thiamine-free medium and dialyzed serum. Normal fibroblasts survived indefinitely without supplemental thiamine, whereas patient cells died in 5-14 days (mean 9.5 days), and heterozygous cells survived for more than 30 days. TRMA fibroblasts were rescued from death with 10-30 nM thiamine (in the range of normal plasma thiamine concentrations). Positive terminal deoxynucleotide transferase-mediated dUTP nick end-labeling (TUNEL) staining suggested that cell death was due to apoptosis. We assessed cellular uptake of [3H]thiamine at submicromolar concentrations. Normal fibroblasts exhibited saturable, high-affinity thiamine uptake (Km 400-550 nM; Vmax 11 pmol/min/10(6) cells) in addition to a low-affinity unsaturable component. Mutant cells lacked detectable high-affinity uptake. At 30 nM thiamine, the rate of uptake of thiamine by TRMA fibroblasts was 10-fold less than that of wild-type, and cells from obligate heterozygotes had an intermediate phenotype. Transfection of TRMA fibroblasts with the yeast thiamine transporter gene THI10 prevented cell death when cells were grown in the absence of supplemental thiamine. We therefore propose that the primary abnormality in TRMA is absence of a high-affinity thiamine transporter and that low intracellular thiamine concentrations in the mutant cells cause biochemical abnormalities that lead to apoptotic cell death.
Figures



Similar articles
-
The gene mutated in thiamine-responsive anaemia with diabetes and deafness (TRMA) encodes a functional thiamine transporter.Nat Genet. 1999 Jul;22(3):305-8. doi: 10.1038/10379. Nat Genet. 1999. PMID: 10391222
-
Defective RNA ribose synthesis in fibroblasts from patients with thiamine-responsive megaloblastic anemia (TRMA).Blood. 2003 Nov 15;102(10):3556-61. doi: 10.1182/blood-2003-05-1537. Epub 2003 Jul 31. Blood. 2003. PMID: 12893755
-
A novel mutation in the SLC19A2 gene in a Tunisian family with thiamine-responsive megaloblastic anaemia, diabetes and deafness syndrome.Br J Haematol. 2001 May;113(2):508-13. doi: 10.1046/j.1365-2141.2001.02774.x. Br J Haematol. 2001. PMID: 11380424
-
Thiamine-responsive megaloblastic anemia syndrome: a disorder of high-affinity thiamine transport.Blood Cells Mol Dis. 2001 Jan-Feb;27(1):135-8. doi: 10.1006/bcmd.2000.0356. Blood Cells Mol Dis. 2001. PMID: 11358373 Review.
-
Recessive SLC19A2 mutations are a cause of neonatal diabetes mellitus in thiamine-responsive megaloblastic anaemia.Pediatr Diabetes. 2012 Jun;13(4):314-21. doi: 10.1111/j.1399-5448.2012.00855.x. Epub 2012 Feb 27. Pediatr Diabetes. 2012. PMID: 22369132 Review.
Cited by
-
An Italian case series' description of thiamine responsive megaloblastic anemia syndrome: importance of early diagnosis and treatment.Ital J Pediatr. 2023 Nov 30;49(1):158. doi: 10.1186/s13052-023-01553-1. Ital J Pediatr. 2023. PMID: 38037112 Free PMC article.
-
SLC19: the folate/thiamine transporter family.Pflugers Arch. 2004 Feb;447(5):641-6. doi: 10.1007/s00424-003-1068-1. Epub 2003 May 6. Pflugers Arch. 2004. PMID: 14770311 Review.
-
Dyserythropoiesis and myelodysplasia in thiamine-responsive megaloblastic anemia syndrome.Clin Case Rep. 2020 Mar 6;8(6):991-994. doi: 10.1002/ccr3.2791. eCollection 2020 Jun. Clin Case Rep. 2020. PMID: 32577249 Free PMC article.
-
Case Report: Genetic and Clinical Features of Maternal Uniparental Isodisomy-Induced Thiamine-Responsive Megaloblastic Anemia Syndrome.Front Pediatr. 2021 Mar 19;9:630329. doi: 10.3389/fped.2021.630329. eCollection 2021. Front Pediatr. 2021. PMID: 33816400 Free PMC article.
-
Cochlear implant and thiamine-responsive megaloblastic anemia syndrome.Ann Saudi Med. 2014 Jan-Feb;34(1):78-80. doi: 10.5144/0256-4947.2014.78. Ann Saudi Med. 2014. PMID: 24658560 Free PMC article.
References
-
- Rogers LE, Porter FS, Sidbury JBJ. Thiamine-responsive megaloblastic anemia. J Pediatr. 1969;74:494–504. - PubMed
-
- Raz T, et al. Refined mapping of the gene for thiamine-responsive megaloblastic anemia syndrome in a 4 cM region and evidence for genetic homogeneity. Hum Genet. 1998;103:455–461. - PubMed
-
- Rotoli B, Poggi V, De Renzo A, Robledo R. In vitro addition of thiamin does not restore BFU-E growth in thiamin-responsive anemia syndrome. Haematologica. 1986;71:441–443. - PubMed
-
- Poggi V, et al. Thiamin-responsive megaloblastic anaemia: a disorder of thiamin transport? J Inherit Metab Dis. 1984;7:153–154. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Molecular Biology Databases

